Volume 13, Issue 1 (Winter 2025)
PCP 2025, 13(1): 57-70 |
Back to browse issues page
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Shiri E, Pouretemad H, Behzadpoor S. The Effectiveness of Family-based Behavior Therapy on Behavioral Excesses of Children With Autism Via Telehealth. PCP 2025; 13 (1) :57-70
URL: http://jpcp.uswr.ac.ir/article-1-954-en.html
URL: http://jpcp.uswr.ac.ir/article-1-954-en.html
1- Department of Psychology, Faculty of Social Sciences, Imam Khomeini International University, Ghazvin, Iran.
2- Institute for Cognitive & Brain Sciences, Shahid Beheshti University, Tehran, Iran.
3- Department of Psychology, Faculty of Humanities, University of Science and Culture, Tehran, Iran. ,samaneh_behzadpoor@yahoo.com
2- Institute for Cognitive & Brain Sciences, Shahid Beheshti University, Tehran, Iran.
3- Department of Psychology, Faculty of Humanities, University of Science and Culture, Tehran, Iran. ,
Keywords: Family-based management of behavioral excesses of autism program (FMBEAP), Behavioral excesses, Autism spectrum disorders (ASD), Telehealth
Full-Text [PDF 679 kb]
(503 Downloads)
| Abstract (HTML) (2579 Views)
Full-Text: (404 Views)
Introduction
Autism spectrum disorder (ASD) is a neurodevelopmental condition characterized by behavioral deficits with behavioral excesses (American Psychiatric Association, 2013). Behavioral excesses, including stereotyped behaviors, repetitive manipulation of objects, self-injurious behaviors, rituals and routines, insisting on consistencies, and restricted interests (Leekam et al., 2011; Szatmari et al., 2006), hurt the children and their families. These behaviors cause problems entering the social and educational environment (Bello-Mojeed et al., 2013; Sigafoos et al., 2009) and limit the child's opportunities to learn new skills (Loftin et al., 2008; Pierce & Courchesne, 2001). Additionally, behavioral excesses usually impede treating behavioral deficits (Matson et al., 2010) and make caregivers feel stressed (Baker-Ericzén et al., 2005; Bello-Mojeed et al., 2013; Lecavalier et al., 2006). If left untreated, behavioral excesses in ASD may persist over time (Baker et al., 2003).
Parent-based interventions seem to be one of the most effective ways to increase access to empirically supported interventions for ASD symptoms (Bagherian Khosroshahi et al., 2010; Brookman-Frazee et al., 2006; Graziano & Diament, 1992). Also, many parent-based interventions on behavioral excesses have been developed in different countries, and their effectiveness has been confirmed (Boyd et al., 2012; Carter et al., 2011; Grahame et al., 2015; Green et al., 2010; Shiri et al., 2020). However, there seem to be many barriers to delivering family-based intervention, especially in developing and developed countries. Some of these barriers include the shortage of eligible therapists, the scarcity of care services and resources, especially in rural and underserved areas, the low economic status of many families, and lengthy waiting lists (Belfer & Saxena, 2006; Taylor et al., 2008; Wainer & Ingersoll, 2015). Thus, it is necessary to determine new ways to provide adequate and appropriate intervention programs for families of children with ASD (Symon, 2001; Wainer & Ingersoll, 2015).
A possible solution to eliminate the mentioned barriers and facilitate the provision of services for families with ASD is telehealth technology (Simacek et al., 2017). Telehealth refers to using communication technologies, like video conferencing, digital discs, mobile applications, telephone, three-dimensional interactive programs, and web-based tutorials. This technology enables providing healthcare services and educational interventions remotely and over various geographical distances (Dudding, 2009; Turner, 2003; Vismara et al., 2012).
Due to the substantial increase in the use of technology, including computers and the internet, in daily life, telehealth services can be an effective and alternative method to provide services and support to families of children with ASD (Rayner et al., 2009; Wainer & Ingersoll, 2015).
Therefore, it can provide families of children with ASD with easy access to cost-effective and efficient intervention and trained professionals. Evidence on telehealth-based parent training indicated that the parents found the programs practical, convenient, and useful (Hamad et al., 2010; Howroyd & Peeters, 2007; Jang et al., 2012).
Previous research has shown telehealth to be a promising and effective intervention method for remotely training parents to manage behavioral excesses of their children with ASD in their homes (Lindgren et al., 2016). Wacker et al. used telehealth services to provide functional communication training (FCT) via telehealth and indicated that this kind of training can reduce behavioral problems in children with ASD and is also acceptable to parents (Wacker et al., 2013; Wacker et al., 2013). Similarly, Suess et al. (2016) examined the parents' fidelity to FCT when is conducted via telehealth in their home. In this line, the results from the pilot trial of Bearss et al. (2015) indicated the feasibility and efficacy of the parent training program for children with ASD and disruptive behaviors when provided via telehealth. This evidence supports the promise and effectiveness of telehealth as an intervention modality for core symptoms and co-occurring behavioral problems in individuals with ASD. Despite these promising results in developed countries, fewer studies have been conducted in developing countries, such as Iran, to use telehealth for the treatment of children with ASD.
Moreover, every intervention for ASD includes some specific expectations and values in its goals and techniques. If these values and expectations match those of the families receiving the intervention, positive therapy outcomes, including high levels of participation and response to treatment, are likely (Benish et al., 2011; Castro et al., 2010; Vigil & Hwa-Froelich, 2004). Therefore, adapting interventions to the family context may be necessary to achieve therapy goals (Castro et al., 2010; Magaña et al., 2017). In addition, immigrant families of children with ASD report that language barriers also influence their ability to build relationships with therapists (Iland et al., 2012; Zetlin et al., 1996). Also, some evidence shows that treatment outcomes may be better (Sue, 1998; Sue et al., 1991). when clients see therapists of the same linguistic background (Sue, 1998; Sue et al., 1991). Telehealth can effectively provide intervention for families who have immigrated to other countries with different contexts. Also, through this method, these families can form therapeutic relationships with a therapist from the same cultural and linguistic background.
Regarding the negative impacts of behavioral excesses on children and their families and the lack of appropriate and effective intervention programs to reduce these behaviors in Iranian children with ASD, a family-based management of behavioral excesses of autism program (FMBEAP) was developed (Shiri et al., 2020). In our previous study, we showed that FMBEAP was a feasible, acceptable, and effective intervention to reduce behavioral excesses in children with ASD when delivered in clinical settings by trained therapists (Shiri et al., 2020). This study is an effort to move those center-based procedures into the families' homes, using video-conferencing. The study predicted that telehealth delivery of FMBEAP would be feasible and effective with families in their homes.
Materials and Methods
Sample and study design
This study is a quasi-experimental design without a control group. All procedures were approved by the Ethical Committee of Shahid Beheshti University. Fourteen families of Iranian children with ASDs referred to the Tehran Autism Center participated in this study. The inclusion criteria included children with the diagnosis of ASD confirmed by at least a consultant clinical psychologist and a child psychiatrist, children at the ages of 2 and 5 years, children without receiving any other treatment during the intervention, the family’s tendency to participate in this study, and families easy access to high-speed internet services and video-conferencing apps, such as Skype and IMO. The exclusion criteria included any evidence for other severe psychological or neurological disorders besides the diagnosis of ASD in children and lack of family cooperation with the therapist during the intervention (such as unexcused absence of more than one session). The parents received FMBEAP via telehealth during ten weekly core sessions and one follow-up session (one month after the end of the intervention).
Measures
Demographic data form
The authors developed a demographic data form to collect demographic information of parents and children. This form contained information about a child’s age and gender, as well as parents’ age, level of education, and employment status, and was completed by parents in the baseline.
Vineland adaptive behavior scales (VABS)
The VABS is commonly used to evaluate some domains of adaptive behavior, including communication, daily living skills, socialization, and motor skills, based on parental reports of a child’s behavior observed in a natural context (VABS) (Sparrow et al., 1985). Tavakoli et al. have standardized this tool in Iran, which has good validity and reliability (Tawakoli et al., 2000). The questionnaire was completed via interviewing parents by a trained psychologist in the baseline.
Stanford-Binet intelligence scale (SB-5)
The SB-5 consists of non-verbal and verbal subtests. It measures a child’s intelligence through five factors, including fluid reasoning, knowledge, quantitative reasoning, visual-spatial processing, and working memory. Roid in 2003 standardized this scale (Roid, 2003). Afrooz and Kamkari (2016) have standardized this test in Iran, and has good validity and reliability (Afrooz & Kamkari, 2016). The SB-5 was administered in the clinic by a trained research psychologist at the baseline.
Repetitive behavior scale-revised (RBS-R)
The RBS-R consists of 43 items across 6 subscales, including self-injurious, stereotyped, routine, compulsions, sameness, and restricted behavior. Items are rated on a four-point Likert scale ranging from [0] “never” to [3] “always” (Bodfish et al., 2000). Also, Ghorban et al (2013) in Iran found the validity of the revised scale of stereotyped behaviors using Cronbach’s α coefficient for the whole scale to be 92%, and by calculating the correlation of the whole scale and its subscales, its construct validity was 68%. 0% to 98% have been reported.
Aberrant behavior checklist (ABC)
The ABC is a parent-report measure containing 58 items. It includes five subscales: Irritability (aggression, tantrums, and self-harm behaviors, 15 items), lethargy/social withdrawal (16 items), stereotypic behaviors (7 items), hyperactivity/noncompliance (16 items), and inappropriate speech (4 items). Each item is rated on a four-point Likert scale from 0 to 3, with higher scores showing greater severity (Aman et al., 1985). Shiri et al., (2020) has standardized this tool in Iran and it is valid and reliable.
Clinical global impression-improvement scale
The clinical global impression-improvement scale assesses improvement or change in patients. It allows the clinician to rate how much the symptoms have worsened or improved relative to the baseline state. The scale’s ratings are 1=very much improved, 2=much improved, 3=minimally improved, 4=not changed, 5=minimally worse, 6=much worse, and 7=very much worse. Some clinicians blind to the study assessed the global response to intervention based on available information, including RBS-R, VABS, and ABC. Ratings of 1 and 2 were considered as ‘improvement’ (Grahame et al., 2015). This measure was used in the post-test.
Parental self-efficacy measure (PSAM)
The PSAM assesses three main domain of parental self-efficacy, including parents’ perception of their parental abilities, their assurance about their successful function regarding paternal roles, and their perception of their ability to manage their children’s behavior (Dumka et al., 1996) middle-income, Anglo mothers (n=90). The reliability obtained for positive parenting self-efficacy showed Cronbach’s α equal to 69%, negative parenting self-efficacy equal to alpha of 65%, and total parenting self-efficacy alpha of 54% (Abareshi et al., 2009).
Therapy attitude inventory (TAI)
The TAI is a 10-item consumer satisfaction measure used to measure parent satisfaction with the process and outcome of the intervention. Parents rated items on a five-point scale from 1 (dissatisfaction with therapy or weakening of symptoms) to 5 (satisfaction with therapy or improvement of symptoms). The score is between 10 and 50. Parents completed this post-treatment inventory. Mohajeri et al. translated and validated this questionnaire for the first time in Iran (Mohajeri et al., 2013). Cronbach’s α of this tool in the present study was 82%.
Telehealth satisfaction survey
The telehealth satisfaction survey was designed for this study to assess parents’ feedback on the telehealth delivery of the FMBEAP program. Questions included therapist-client interaction, the usefulness of the telehealth equipment, and satisfaction with the teledelivery of the FMBEAP via telehealth. Responses were rated on a five-point Likert scale from 1 (strongly disagree) to 5 (strongly agree). The lowest score in this questionnaire was 21, and the highest was 105. The score for each participant is obtained by the sum of scores across all items divided by 105×100. In this study, parents completed a post-treatment inventory.
Treatment fidelity
Two independent raters were randomly allocated 10% of the recorded intervention sessions to rate the fidelity to the program manual to assess the fidelity to intervention using a checklist (Johnson et al., 2007). Raters rated fidelity to the manual of each session using a three-point scale from 0 (objectives of parents/therapist are not achieved) to 2 (objectives of parents/therapist are fully achieved).
Study procedure
Parents of children with the inclusion criteria were invited to the study. Before the intervention, the research process and how to use the video-conferencing apps was explained to families via telephone. Then, families completed initial assessments. The expert psychologist delivered intervention in ten weekly sessions of 90 minutes via telehealth. The sessions were held in 3 or 4 families in each group. An educational booklet on the content of treatment sessions was provided and sent to the families by e-mail. After each session, families presented a report about implementing the treatment strategies, and the therapist guided them to solve possible problems. Assessments also took place immediately at the end of the intervention (10 weeks) and one month after the end of the intervention. All assessments were administered by the trained research psychologist blinded to the study.
Intervention
FMBEAP is a group therapy focusing on helping parents use the ABA framework to prevent or overcome behavioral excesses of their children within the context of daily life. This therapy is designed to teach parents the following skills, to classify the lower and higher-order behavioral excesses of children with ASD and their effects on the family and the child, to identify the antecedent and consequence of behavioral excesses, and to design effective therapeutic strategies to prevent and manage these behaviors, to engage the child with many pre-programmed interactions with the theme of pleasure activities, and to apply the therapeutic techniques across the waking time of the child by caregivers. FMBEAP contains ten weekly core sessions and one follow-up session one month after the end of the intervention. Additionally, the weekly assignment was given to parents. A copy of the program is available with the corresponding author. This program was designed based on Johnson et al., (2007) manual. In the first session, some primary information was introduced, including behavioral excesses definitions and associated impairments, the role of the parent in treatment, the content of the program, and treatment goals. The second session clarified the basic principles of applied behavior analysis (ABA) (antecedent, behavior, consequent). In the third and fourth sessions, prevention strategies were trained, such as modifying the child’s environment or activities and engaging the child with a wide range of pre-programmed interactions. In the fifth session, the parents were taught to promote and train their children to do adaptive behaviors instead of behavioral excesses. In the sixth session, the principles of reinforcement and the usage of reinforcement to increase positive behaviors in children were discussed. In the seventh session, the extinction strategies and response cost procedures were considered. In the eighth session, differential reinforcement and response interruption and redirection techniques were trained. In the ninth and tenth sessions, functional communication skills and strategies for generalization and maintenance were focused, respectively (Shiri et al., 2020).
Data analysis
Data were analyzed using repeated measures analysis of variance (ANOVA) and the least significant differences (LSD) post hoc test with the SPSS software, version 21.
Results
Socio-demographic characteristics
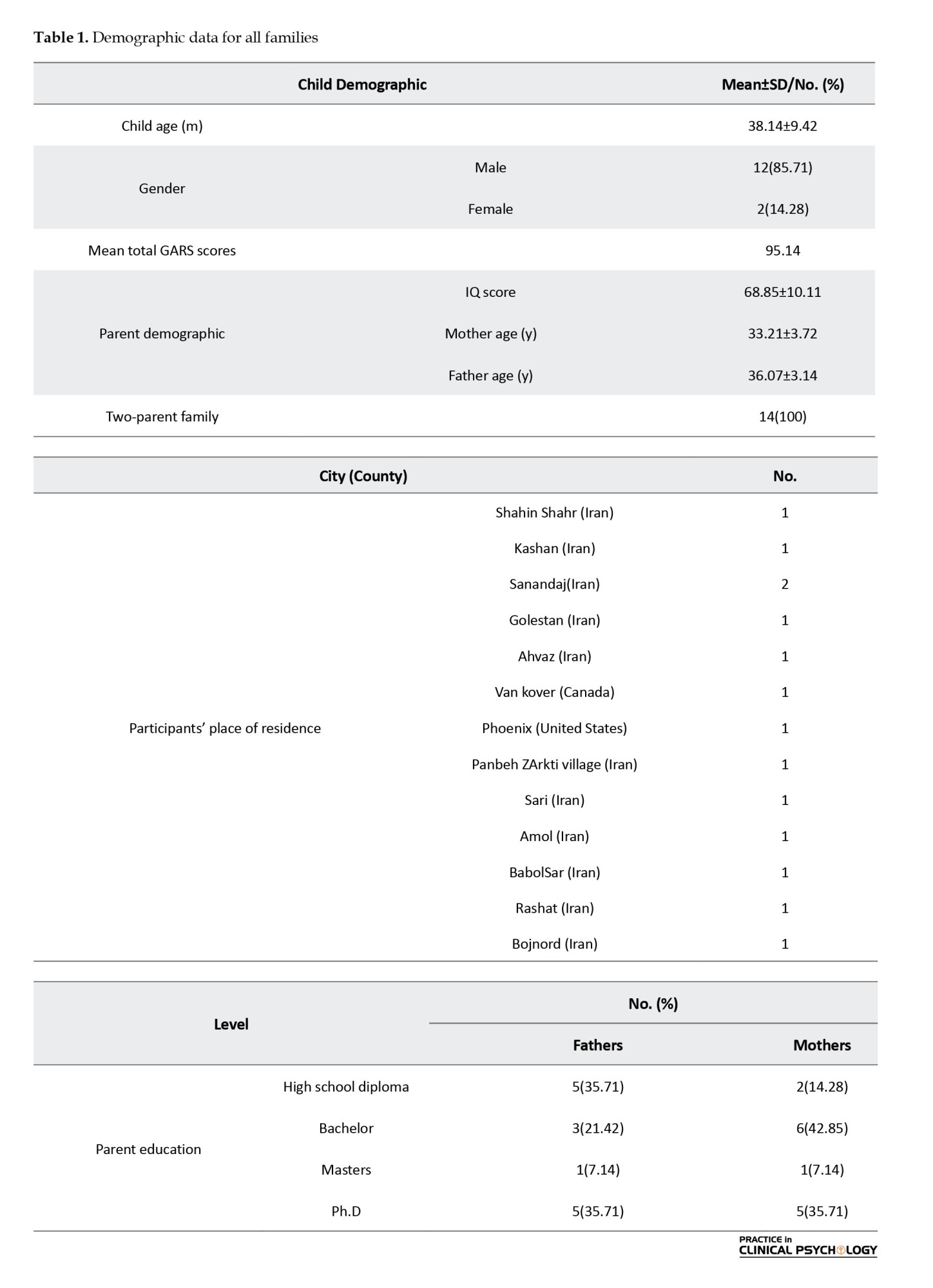
As indicated in Table 1, 2 children were girls and 12 were boys. All children were diagnosed with ASD. Intelligence quotients (IQs) ranged from 51 to 86, and 42% of children had an intellectual disability (IQ<70) (Table 1).
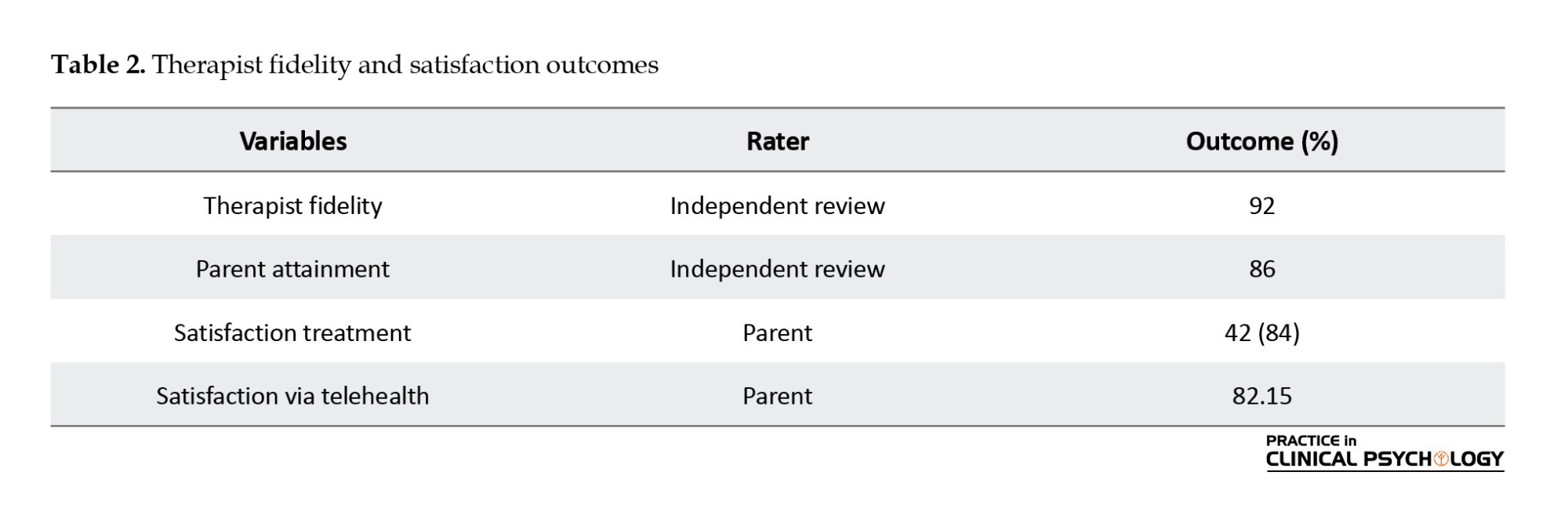
Therapist fidelity and satisfaction outcomes
Based on the independent evaluation of 10% of randomly selected therapy sessions, the therapist’s fidelity to the protocol was 92%, and the parent attained about 86% of therapy objectives. The Mean±SD parent satisfaction score with treatment was 41.22±8.45. Also, the Mean±SD score of parent satisfaction with the delivery of FMBEAP via telehealth was 84.33±7.87. Parents were positive toward the intervention and its delivery via telehealth (Table 2).
Efficacy outcomes
Behavioral excesses
Repeated measures ANOVA was used to examine the significance of changes in the behavioral excesses of children with ASD. Table 3 presents the mean and standard deviation of the behavioral excesses at three time points, including pre-test, post-test, and follow-up. Table 3 also presents the results of repeated measures ANOVA. Statistically significant reductions were observed in RBS-R’s subscales from pre-test to post-test and post-test to follow-up, with an effect size ranging from 0.30 to 0.72 (Table 3).
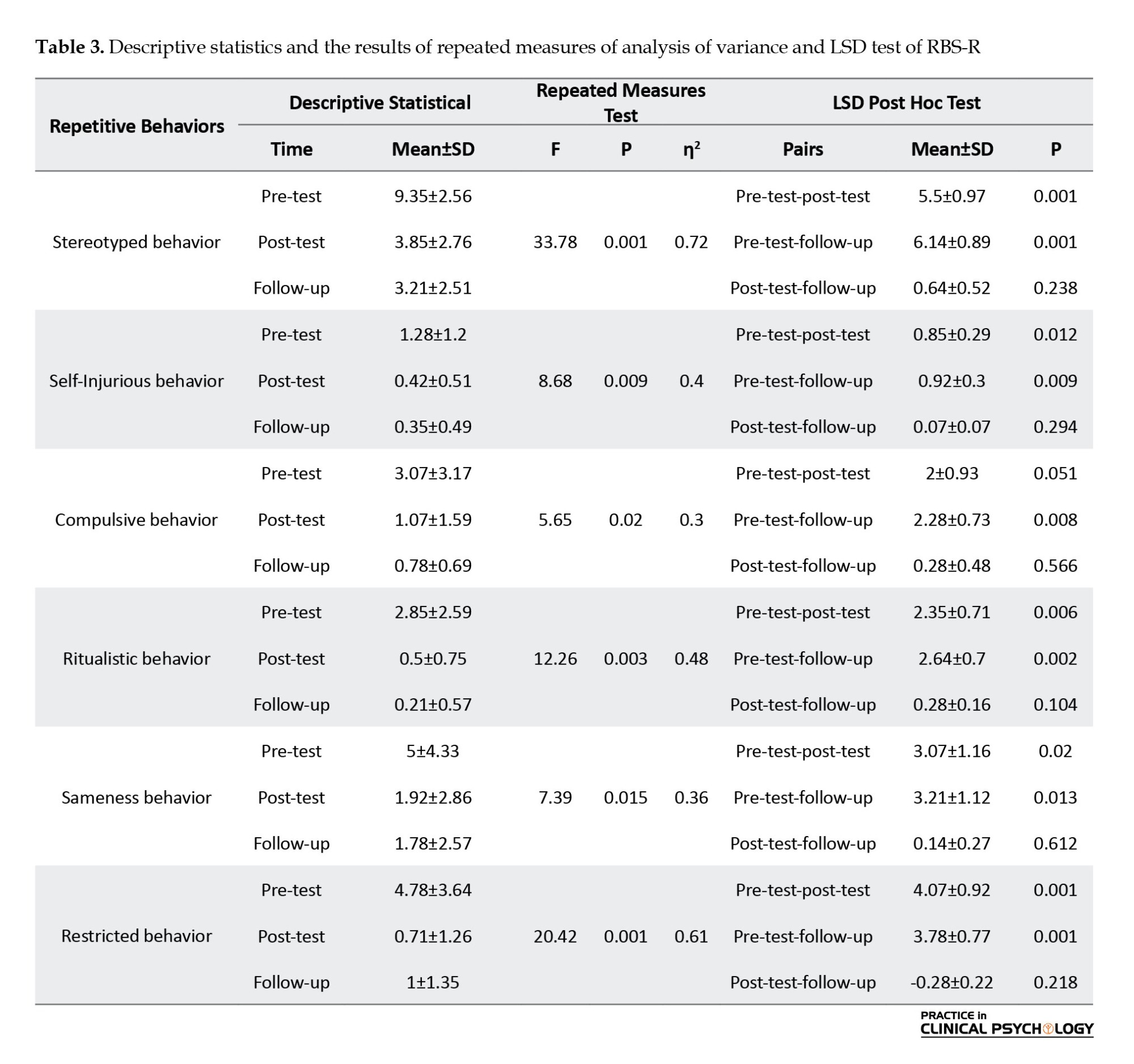
Table 3 presents the results of the post hoc analysis using the LSD test for multiple comparisons. As shown in Table 3, stereotyped behaviors, self-injurious behaviors, compulsive behaviors, ritualistic behaviors, sameness behaviors, and restricted behaviors have significantly decreased in the post-test and follow-up stages. This result showed that the effects of the treatment were sustained even four months after the end of the intervention.
Table 4 presents the results of repeated measures to investigate the effect of FMBEAP on the ABC checklist. Analyses on the ABC checklist indicated that behavioral excesses were significantly decreased in the post-test and follow-up stages compared to the baseline (Table 4).
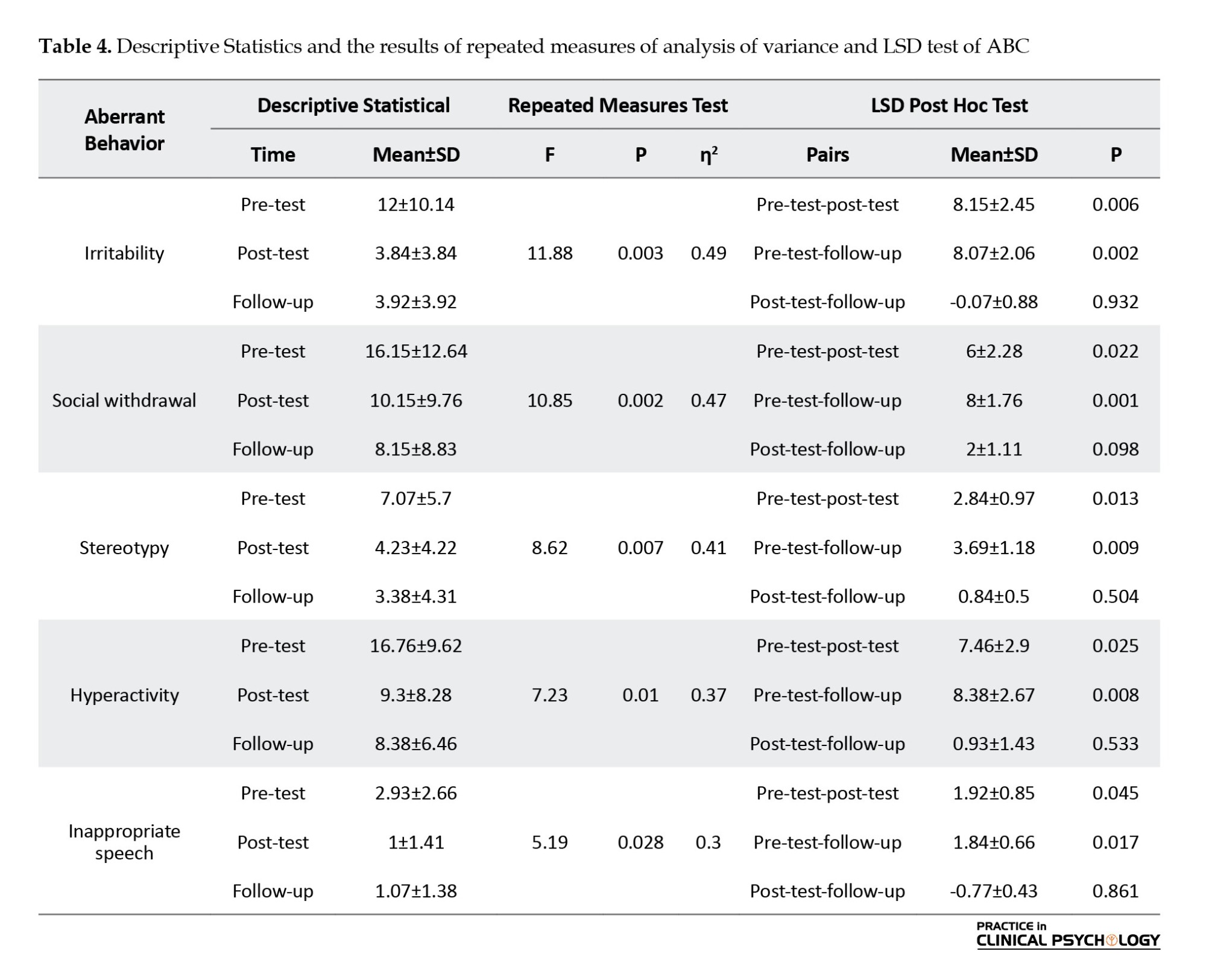
Table 4 presents the results of the post hoc test and paired comparison and Table 4 presents the results of the LSD for multiple comparisons. According to Table 4, in the post-test and follow-up stages, irritability, social withdrawal, stereotypy, hyperactivity, and inappropriate speech significantly decreased compared to the baseline. These results indicated that the effects of FMBEAP were sustained even four months after the end of the intervention. Data analysis suggests FMBEAP has a significant effect on behavioral excesses of children with ASD with an acceptable effect size.
In addition, the results indicated that 12 participants (85%) were rated as much improved (n=5) or very much improved (n=7) on the blind rating of CGI-I. Two participants (15%) met minimally improved and no change criteria.
Parent self-efficacy
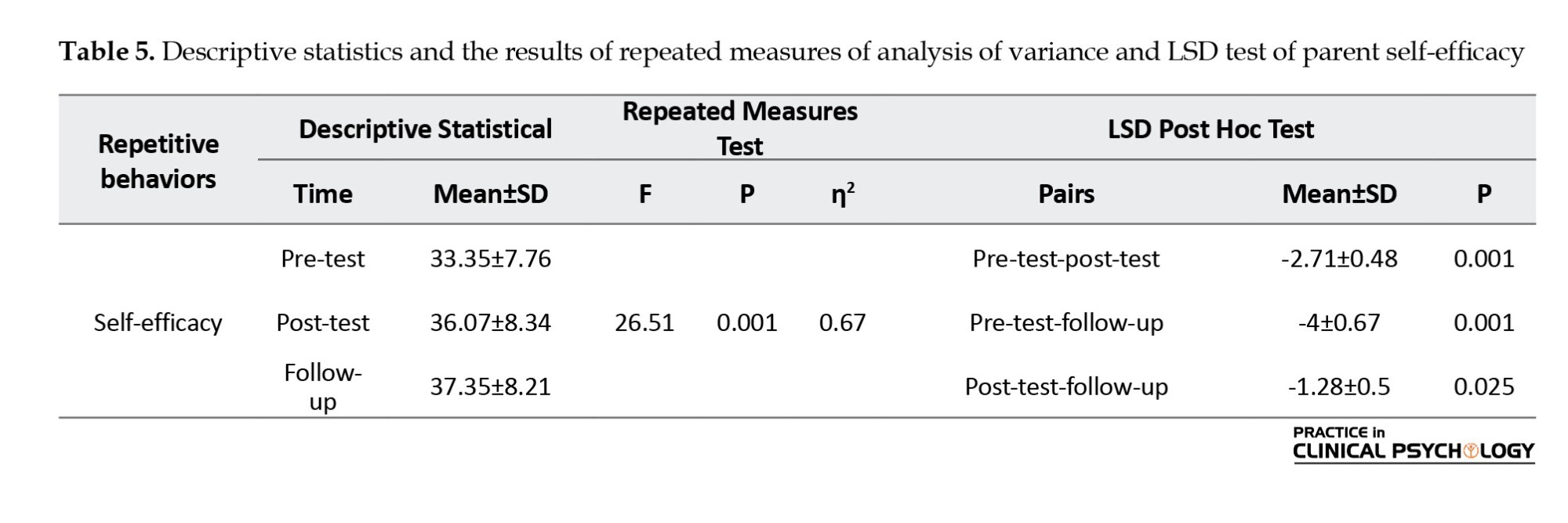
The results of repeated measures showed a significant change over time in parent self-efficacy. They demonstrated that parent self-efficacy increased in the post-test and follow-up stages compared to the baseline (Table 5).
Multiple comparisons using the LSD method showed that parent self-efficacy increased in the post-test and follow-up stages compared to the baseline. These results indicated that changes in parent self-efficacy have been sustained over time.
Discussion
This study’s results support the acceptability, feasibility, and preliminary efficacy of FMBEAP to reduce behavioral excesses in children with ASD when delivered via telehealth. The program was acceptable to parents, evidenced by an 82.15 satisfaction rate and 86% attainment of session goals. Therapists consistently delivered the program, evidenced by 92% fidelity on a sample of sessions evaluated by independent reviewers.
The results are consistent with those from a recent randomized clinical trial by (Shiri et al., 2020).The results of the present study indicated that even with required modifications to the original manual (e.g. deletion of the home visit and role-play), FMBEAP can be provided reliably for parents via telehealth with high rates of acceptance and satisfaction. The results of the current study confirmed the results reported by Bearss et al. (2018), (Barretto et al. (2006), Wacker et al., (2013), and Suess et al. (2016) we provided a demonstration of the use of telehealth to assess and initiate treatment of problem behavior in an outpatient clinic. We coached parents of children with autism via telehealth to conduct functional analyses during 1 appointment that lasted 1 hr and subsequently coached them as they implemented FCT during 3 subsequent appointments (15 min each and indicated that behavioral treatments to reduce behavioral excesses could be provided effectively via telehealth. In one of the most recent studies evaluating the feasibility of parent training to reduce behavioral excesses delivered via telehealth, Bearss et al. (2018) reported that disruptive behavior was reduced by an average of 78.6% for 14 children with ASDs. Also, this behavioral intervention via telehealth was acceptable to caregivers. In this line, the results provided by Suess et al. (2016) indicated that caregivers could implement behavioral techniques with acceptable fidelity when supervised by a therapist via telehealth.
However, the children and families in this telehealth study substantially differed from our previous study via direct supervision (Shiri et al., 2020). For example, 42% of children had intellectual disabilities (IQ<70) compared to 30% in the previous trial. In our previous trial, 100% of mothers and 82% of fathers had college or advanced degrees compared to 65% of fathers and 86% of mothers participating in this telehealth trial. Additionally, all the families in our previous study lived in Tehran City (the capital of Iran), but the families participating in this study lived in different cities and rural sites of Iran, and 2 of them were Iranian immigrants living in Canada and the United States. Demonstrating the efficacy and feasibility of FMBEAP by telehealth in a diverse sample of families with different socioeconomic statuses is a small but crucial step toward administrating an evidence-based intervention for families who lack access to behavioral services. Also, by delivering the intervention to families via telehealth, many barriers and challenges related to travel, cost of service delivery, and availability of trained therapists may be alleviated. Furthermore, the effectiveness of FMBEAP via telehealth for immigrant families suggests that this modality of service delivery can be effectively used for those families.
In FMBEAP, parents were trained to identify the antecedents and consequences of children’s behavior. Therefore they could analyze these behaviors and design appropriate and effective strategies to reduce them. They were also thought to enrich the child’s environment and engage them in appropriate activities that, in turn, could reduce the time that children engage in behavioral excesses (Shiri et al., 2020). Parents performed all these therapeutic techniques throughout the child’s waking hours, which may be the main reason for the high efficacy of FMBEAP. The secondary gain of this intervention was an improvement in parent’s self-efficacy. When parents learn how to manage their child’s behaviors and reduce their child’s behavioral excess, their self-efficacy increases. The results showed that parents can learn all these procedures with high acceptability via telehealth. Thus, telehealth can be a valuable method to deliver behavioral treatments to reduce behavioral excesses in children with ASD with acceptable fidelity.
However, if telehealth is to become a viable method for providing services to families, some prerequisites are necessary, including familiarity with internet-based technology, access to high-speed internet, motivation to participate in treatment, and careful implementation of the intervention strategies.
The current study adds to the empirical evidence for the validity of telehealth service-delivery models, but it has several limitations. The fundamental limitation is the lack of a control group. The absence of a control group makes it impossible to separate the effects of the intervention from the effects of other factors, including regression to mean, time or attention on behavioral excesses, and practice effect. Also, the small sample size limits the generalizability of results. Finally, some measures of the study were filled out by the parents, who were not blinded to the purpose of the study.
The results of this study provided support for the feasibility, acceptability, and efficacy of parent-mediated interventions via telehealth to decrease the behavioral excesses of children with ASD. Additionally, we found that providing training to parents from a distance via video-conferencing technology is an effective and valuable service delivery modality. Given the limitations of this study, further large-scale trials controlling for unrelated factors, and measurement-blind approaches are needed to evaluate the reliability of FMBEAP via telehealth. It is also suggested that the effectiveness of FMBEAP via telehealth be tested in a large sample of immigrant families. Additionally, future issues regarding the delivery of parent-implemented intervention via telehealth should focus on strategies most likely to increase parent’s motivation to engage in online interventions. Finally, telehealth is suggested as a valuable method to deliver psychological services to families of children with ASD in some crisis conditions, including infectious disease outbreaks that necessitate social distancing and staying home.
Conclusion
Taken together, the results of this study provide support for feasibility, acceptability, and efficacy of parent-mediated interventions via telehealth to decrease the behavioral excesses of children with ASD. Additionally, we found that providing training to parents from a distance via video-conferencing technology was an effective and useful modality of service delivery. Given the limitations of this study, further large-scale trials controlling for unrelated factors, as well as blinded approaches to measurement, is needed to evaluate the reliability of FMBEAP via telehealth. It is also suggested to test the effectiveness of FMBEAP via telehealth in a large sample of immigrant families. Additionally, future issues regarding the delivery of parent-implemented intervention via telehealth will need to focus on which strategies are most likely to increase parent’s motivation to engage in online interventions. Finally, thelehealth is suggested as a useful method to deliver psychological services to families of children with ASD in some crisis conditions including infectious disease outbreaks that necessitate social distancing and staying home.
Ethical Considerations
Compliance with ethical guidelines
This study was approved by the Ethical Committee of Shahid Beheshti University, Tehran, Iran (Code: IR. ISB. ICBS. 97/1013).
Funding
This research did not receive any grant from funding agencies in the public, commercial, or non-profit sectors.
Authors' contributions
All authors equally contributed to preparing this article.
Conflict of interest
The authors declared no conflict of interest.
Acknowledgments
The authors thank the Center of Excellence in Cognitive Neuropsychology, Institute for Cognitive and Brain Sciences, Shahid Beheshti University, Tehran, Iran, and all the children and parents who participated in this study.
References
Autism spectrum disorder (ASD) is a neurodevelopmental condition characterized by behavioral deficits with behavioral excesses (American Psychiatric Association, 2013). Behavioral excesses, including stereotyped behaviors, repetitive manipulation of objects, self-injurious behaviors, rituals and routines, insisting on consistencies, and restricted interests (Leekam et al., 2011; Szatmari et al., 2006), hurt the children and their families. These behaviors cause problems entering the social and educational environment (Bello-Mojeed et al., 2013; Sigafoos et al., 2009) and limit the child's opportunities to learn new skills (Loftin et al., 2008; Pierce & Courchesne, 2001). Additionally, behavioral excesses usually impede treating behavioral deficits (Matson et al., 2010) and make caregivers feel stressed (Baker-Ericzén et al., 2005; Bello-Mojeed et al., 2013; Lecavalier et al., 2006). If left untreated, behavioral excesses in ASD may persist over time (Baker et al., 2003).
Parent-based interventions seem to be one of the most effective ways to increase access to empirically supported interventions for ASD symptoms (Bagherian Khosroshahi et al., 2010; Brookman-Frazee et al., 2006; Graziano & Diament, 1992). Also, many parent-based interventions on behavioral excesses have been developed in different countries, and their effectiveness has been confirmed (Boyd et al., 2012; Carter et al., 2011; Grahame et al., 2015; Green et al., 2010; Shiri et al., 2020). However, there seem to be many barriers to delivering family-based intervention, especially in developing and developed countries. Some of these barriers include the shortage of eligible therapists, the scarcity of care services and resources, especially in rural and underserved areas, the low economic status of many families, and lengthy waiting lists (Belfer & Saxena, 2006; Taylor et al., 2008; Wainer & Ingersoll, 2015). Thus, it is necessary to determine new ways to provide adequate and appropriate intervention programs for families of children with ASD (Symon, 2001; Wainer & Ingersoll, 2015).
A possible solution to eliminate the mentioned barriers and facilitate the provision of services for families with ASD is telehealth technology (Simacek et al., 2017). Telehealth refers to using communication technologies, like video conferencing, digital discs, mobile applications, telephone, three-dimensional interactive programs, and web-based tutorials. This technology enables providing healthcare services and educational interventions remotely and over various geographical distances (Dudding, 2009; Turner, 2003; Vismara et al., 2012).
Due to the substantial increase in the use of technology, including computers and the internet, in daily life, telehealth services can be an effective and alternative method to provide services and support to families of children with ASD (Rayner et al., 2009; Wainer & Ingersoll, 2015).
Therefore, it can provide families of children with ASD with easy access to cost-effective and efficient intervention and trained professionals. Evidence on telehealth-based parent training indicated that the parents found the programs practical, convenient, and useful (Hamad et al., 2010; Howroyd & Peeters, 2007; Jang et al., 2012).
Previous research has shown telehealth to be a promising and effective intervention method for remotely training parents to manage behavioral excesses of their children with ASD in their homes (Lindgren et al., 2016). Wacker et al. used telehealth services to provide functional communication training (FCT) via telehealth and indicated that this kind of training can reduce behavioral problems in children with ASD and is also acceptable to parents (Wacker et al., 2013; Wacker et al., 2013). Similarly, Suess et al. (2016) examined the parents' fidelity to FCT when is conducted via telehealth in their home. In this line, the results from the pilot trial of Bearss et al. (2015) indicated the feasibility and efficacy of the parent training program for children with ASD and disruptive behaviors when provided via telehealth. This evidence supports the promise and effectiveness of telehealth as an intervention modality for core symptoms and co-occurring behavioral problems in individuals with ASD. Despite these promising results in developed countries, fewer studies have been conducted in developing countries, such as Iran, to use telehealth for the treatment of children with ASD.
Moreover, every intervention for ASD includes some specific expectations and values in its goals and techniques. If these values and expectations match those of the families receiving the intervention, positive therapy outcomes, including high levels of participation and response to treatment, are likely (Benish et al., 2011; Castro et al., 2010; Vigil & Hwa-Froelich, 2004). Therefore, adapting interventions to the family context may be necessary to achieve therapy goals (Castro et al., 2010; Magaña et al., 2017). In addition, immigrant families of children with ASD report that language barriers also influence their ability to build relationships with therapists (Iland et al., 2012; Zetlin et al., 1996). Also, some evidence shows that treatment outcomes may be better (Sue, 1998; Sue et al., 1991). when clients see therapists of the same linguistic background (Sue, 1998; Sue et al., 1991). Telehealth can effectively provide intervention for families who have immigrated to other countries with different contexts. Also, through this method, these families can form therapeutic relationships with a therapist from the same cultural and linguistic background.
Regarding the negative impacts of behavioral excesses on children and their families and the lack of appropriate and effective intervention programs to reduce these behaviors in Iranian children with ASD, a family-based management of behavioral excesses of autism program (FMBEAP) was developed (Shiri et al., 2020). In our previous study, we showed that FMBEAP was a feasible, acceptable, and effective intervention to reduce behavioral excesses in children with ASD when delivered in clinical settings by trained therapists (Shiri et al., 2020). This study is an effort to move those center-based procedures into the families' homes, using video-conferencing. The study predicted that telehealth delivery of FMBEAP would be feasible and effective with families in their homes.
Materials and Methods
Sample and study design
This study is a quasi-experimental design without a control group. All procedures were approved by the Ethical Committee of Shahid Beheshti University. Fourteen families of Iranian children with ASDs referred to the Tehran Autism Center participated in this study. The inclusion criteria included children with the diagnosis of ASD confirmed by at least a consultant clinical psychologist and a child psychiatrist, children at the ages of 2 and 5 years, children without receiving any other treatment during the intervention, the family’s tendency to participate in this study, and families easy access to high-speed internet services and video-conferencing apps, such as Skype and IMO. The exclusion criteria included any evidence for other severe psychological or neurological disorders besides the diagnosis of ASD in children and lack of family cooperation with the therapist during the intervention (such as unexcused absence of more than one session). The parents received FMBEAP via telehealth during ten weekly core sessions and one follow-up session (one month after the end of the intervention).
Measures
Demographic data form
The authors developed a demographic data form to collect demographic information of parents and children. This form contained information about a child’s age and gender, as well as parents’ age, level of education, and employment status, and was completed by parents in the baseline.
Vineland adaptive behavior scales (VABS)
The VABS is commonly used to evaluate some domains of adaptive behavior, including communication, daily living skills, socialization, and motor skills, based on parental reports of a child’s behavior observed in a natural context (VABS) (Sparrow et al., 1985). Tavakoli et al. have standardized this tool in Iran, which has good validity and reliability (Tawakoli et al., 2000). The questionnaire was completed via interviewing parents by a trained psychologist in the baseline.
Stanford-Binet intelligence scale (SB-5)
The SB-5 consists of non-verbal and verbal subtests. It measures a child’s intelligence through five factors, including fluid reasoning, knowledge, quantitative reasoning, visual-spatial processing, and working memory. Roid in 2003 standardized this scale (Roid, 2003). Afrooz and Kamkari (2016) have standardized this test in Iran, and has good validity and reliability (Afrooz & Kamkari, 2016). The SB-5 was administered in the clinic by a trained research psychologist at the baseline.
Repetitive behavior scale-revised (RBS-R)
The RBS-R consists of 43 items across 6 subscales, including self-injurious, stereotyped, routine, compulsions, sameness, and restricted behavior. Items are rated on a four-point Likert scale ranging from [0] “never” to [3] “always” (Bodfish et al., 2000). Also, Ghorban et al (2013) in Iran found the validity of the revised scale of stereotyped behaviors using Cronbach’s α coefficient for the whole scale to be 92%, and by calculating the correlation of the whole scale and its subscales, its construct validity was 68%. 0% to 98% have been reported.
Aberrant behavior checklist (ABC)
The ABC is a parent-report measure containing 58 items. It includes five subscales: Irritability (aggression, tantrums, and self-harm behaviors, 15 items), lethargy/social withdrawal (16 items), stereotypic behaviors (7 items), hyperactivity/noncompliance (16 items), and inappropriate speech (4 items). Each item is rated on a four-point Likert scale from 0 to 3, with higher scores showing greater severity (Aman et al., 1985). Shiri et al., (2020) has standardized this tool in Iran and it is valid and reliable.
Clinical global impression-improvement scale
The clinical global impression-improvement scale assesses improvement or change in patients. It allows the clinician to rate how much the symptoms have worsened or improved relative to the baseline state. The scale’s ratings are 1=very much improved, 2=much improved, 3=minimally improved, 4=not changed, 5=minimally worse, 6=much worse, and 7=very much worse. Some clinicians blind to the study assessed the global response to intervention based on available information, including RBS-R, VABS, and ABC. Ratings of 1 and 2 were considered as ‘improvement’ (Grahame et al., 2015). This measure was used in the post-test.
Parental self-efficacy measure (PSAM)
The PSAM assesses three main domain of parental self-efficacy, including parents’ perception of their parental abilities, their assurance about their successful function regarding paternal roles, and their perception of their ability to manage their children’s behavior (Dumka et al., 1996) middle-income, Anglo mothers (n=90). The reliability obtained for positive parenting self-efficacy showed Cronbach’s α equal to 69%, negative parenting self-efficacy equal to alpha of 65%, and total parenting self-efficacy alpha of 54% (Abareshi et al., 2009).
Therapy attitude inventory (TAI)
The TAI is a 10-item consumer satisfaction measure used to measure parent satisfaction with the process and outcome of the intervention. Parents rated items on a five-point scale from 1 (dissatisfaction with therapy or weakening of symptoms) to 5 (satisfaction with therapy or improvement of symptoms). The score is between 10 and 50. Parents completed this post-treatment inventory. Mohajeri et al. translated and validated this questionnaire for the first time in Iran (Mohajeri et al., 2013). Cronbach’s α of this tool in the present study was 82%.
Telehealth satisfaction survey
The telehealth satisfaction survey was designed for this study to assess parents’ feedback on the telehealth delivery of the FMBEAP program. Questions included therapist-client interaction, the usefulness of the telehealth equipment, and satisfaction with the teledelivery of the FMBEAP via telehealth. Responses were rated on a five-point Likert scale from 1 (strongly disagree) to 5 (strongly agree). The lowest score in this questionnaire was 21, and the highest was 105. The score for each participant is obtained by the sum of scores across all items divided by 105×100. In this study, parents completed a post-treatment inventory.
Treatment fidelity
Two independent raters were randomly allocated 10% of the recorded intervention sessions to rate the fidelity to the program manual to assess the fidelity to intervention using a checklist (Johnson et al., 2007). Raters rated fidelity to the manual of each session using a three-point scale from 0 (objectives of parents/therapist are not achieved) to 2 (objectives of parents/therapist are fully achieved).
Study procedure
Parents of children with the inclusion criteria were invited to the study. Before the intervention, the research process and how to use the video-conferencing apps was explained to families via telephone. Then, families completed initial assessments. The expert psychologist delivered intervention in ten weekly sessions of 90 minutes via telehealth. The sessions were held in 3 or 4 families in each group. An educational booklet on the content of treatment sessions was provided and sent to the families by e-mail. After each session, families presented a report about implementing the treatment strategies, and the therapist guided them to solve possible problems. Assessments also took place immediately at the end of the intervention (10 weeks) and one month after the end of the intervention. All assessments were administered by the trained research psychologist blinded to the study.
Intervention
FMBEAP is a group therapy focusing on helping parents use the ABA framework to prevent or overcome behavioral excesses of their children within the context of daily life. This therapy is designed to teach parents the following skills, to classify the lower and higher-order behavioral excesses of children with ASD and their effects on the family and the child, to identify the antecedent and consequence of behavioral excesses, and to design effective therapeutic strategies to prevent and manage these behaviors, to engage the child with many pre-programmed interactions with the theme of pleasure activities, and to apply the therapeutic techniques across the waking time of the child by caregivers. FMBEAP contains ten weekly core sessions and one follow-up session one month after the end of the intervention. Additionally, the weekly assignment was given to parents. A copy of the program is available with the corresponding author. This program was designed based on Johnson et al., (2007) manual. In the first session, some primary information was introduced, including behavioral excesses definitions and associated impairments, the role of the parent in treatment, the content of the program, and treatment goals. The second session clarified the basic principles of applied behavior analysis (ABA) (antecedent, behavior, consequent). In the third and fourth sessions, prevention strategies were trained, such as modifying the child’s environment or activities and engaging the child with a wide range of pre-programmed interactions. In the fifth session, the parents were taught to promote and train their children to do adaptive behaviors instead of behavioral excesses. In the sixth session, the principles of reinforcement and the usage of reinforcement to increase positive behaviors in children were discussed. In the seventh session, the extinction strategies and response cost procedures were considered. In the eighth session, differential reinforcement and response interruption and redirection techniques were trained. In the ninth and tenth sessions, functional communication skills and strategies for generalization and maintenance were focused, respectively (Shiri et al., 2020).
Data analysis
Data were analyzed using repeated measures analysis of variance (ANOVA) and the least significant differences (LSD) post hoc test with the SPSS software, version 21.
Results
Socio-demographic characteristics
As indicated in Table 1, 2 children were girls and 12 were boys. All children were diagnosed with ASD. Intelligence quotients (IQs) ranged from 51 to 86, and 42% of children had an intellectual disability (IQ<70) (Table 1).

Therapist fidelity and satisfaction outcomes
Based on the independent evaluation of 10% of randomly selected therapy sessions, the therapist’s fidelity to the protocol was 92%, and the parent attained about 86% of therapy objectives. The Mean±SD parent satisfaction score with treatment was 41.22±8.45. Also, the Mean±SD score of parent satisfaction with the delivery of FMBEAP via telehealth was 84.33±7.87. Parents were positive toward the intervention and its delivery via telehealth (Table 2).

Efficacy outcomes
Behavioral excesses
Repeated measures ANOVA was used to examine the significance of changes in the behavioral excesses of children with ASD. Table 3 presents the mean and standard deviation of the behavioral excesses at three time points, including pre-test, post-test, and follow-up. Table 3 also presents the results of repeated measures ANOVA. Statistically significant reductions were observed in RBS-R’s subscales from pre-test to post-test and post-test to follow-up, with an effect size ranging from 0.30 to 0.72 (Table 3).

Table 3 presents the results of the post hoc analysis using the LSD test for multiple comparisons. As shown in Table 3, stereotyped behaviors, self-injurious behaviors, compulsive behaviors, ritualistic behaviors, sameness behaviors, and restricted behaviors have significantly decreased in the post-test and follow-up stages. This result showed that the effects of the treatment were sustained even four months after the end of the intervention.
Table 4 presents the results of repeated measures to investigate the effect of FMBEAP on the ABC checklist. Analyses on the ABC checklist indicated that behavioral excesses were significantly decreased in the post-test and follow-up stages compared to the baseline (Table 4).

Table 4 presents the results of the post hoc test and paired comparison and Table 4 presents the results of the LSD for multiple comparisons. According to Table 4, in the post-test and follow-up stages, irritability, social withdrawal, stereotypy, hyperactivity, and inappropriate speech significantly decreased compared to the baseline. These results indicated that the effects of FMBEAP were sustained even four months after the end of the intervention. Data analysis suggests FMBEAP has a significant effect on behavioral excesses of children with ASD with an acceptable effect size.
In addition, the results indicated that 12 participants (85%) were rated as much improved (n=5) or very much improved (n=7) on the blind rating of CGI-I. Two participants (15%) met minimally improved and no change criteria.
Parent self-efficacy
The results of repeated measures showed a significant change over time in parent self-efficacy. They demonstrated that parent self-efficacy increased in the post-test and follow-up stages compared to the baseline (Table 5).
Multiple comparisons using the LSD method showed that parent self-efficacy increased in the post-test and follow-up stages compared to the baseline. These results indicated that changes in parent self-efficacy have been sustained over time.

Discussion
This study’s results support the acceptability, feasibility, and preliminary efficacy of FMBEAP to reduce behavioral excesses in children with ASD when delivered via telehealth. The program was acceptable to parents, evidenced by an 82.15 satisfaction rate and 86% attainment of session goals. Therapists consistently delivered the program, evidenced by 92% fidelity on a sample of sessions evaluated by independent reviewers.
The results are consistent with those from a recent randomized clinical trial by (Shiri et al., 2020).The results of the present study indicated that even with required modifications to the original manual (e.g. deletion of the home visit and role-play), FMBEAP can be provided reliably for parents via telehealth with high rates of acceptance and satisfaction. The results of the current study confirmed the results reported by Bearss et al. (2018), (Barretto et al. (2006), Wacker et al., (2013), and Suess et al. (2016) we provided a demonstration of the use of telehealth to assess and initiate treatment of problem behavior in an outpatient clinic. We coached parents of children with autism via telehealth to conduct functional analyses during 1 appointment that lasted 1 hr and subsequently coached them as they implemented FCT during 3 subsequent appointments (15 min each and indicated that behavioral treatments to reduce behavioral excesses could be provided effectively via telehealth. In one of the most recent studies evaluating the feasibility of parent training to reduce behavioral excesses delivered via telehealth, Bearss et al. (2018) reported that disruptive behavior was reduced by an average of 78.6% for 14 children with ASDs. Also, this behavioral intervention via telehealth was acceptable to caregivers. In this line, the results provided by Suess et al. (2016) indicated that caregivers could implement behavioral techniques with acceptable fidelity when supervised by a therapist via telehealth.
However, the children and families in this telehealth study substantially differed from our previous study via direct supervision (Shiri et al., 2020). For example, 42% of children had intellectual disabilities (IQ<70) compared to 30% in the previous trial. In our previous trial, 100% of mothers and 82% of fathers had college or advanced degrees compared to 65% of fathers and 86% of mothers participating in this telehealth trial. Additionally, all the families in our previous study lived in Tehran City (the capital of Iran), but the families participating in this study lived in different cities and rural sites of Iran, and 2 of them were Iranian immigrants living in Canada and the United States. Demonstrating the efficacy and feasibility of FMBEAP by telehealth in a diverse sample of families with different socioeconomic statuses is a small but crucial step toward administrating an evidence-based intervention for families who lack access to behavioral services. Also, by delivering the intervention to families via telehealth, many barriers and challenges related to travel, cost of service delivery, and availability of trained therapists may be alleviated. Furthermore, the effectiveness of FMBEAP via telehealth for immigrant families suggests that this modality of service delivery can be effectively used for those families.
In FMBEAP, parents were trained to identify the antecedents and consequences of children’s behavior. Therefore they could analyze these behaviors and design appropriate and effective strategies to reduce them. They were also thought to enrich the child’s environment and engage them in appropriate activities that, in turn, could reduce the time that children engage in behavioral excesses (Shiri et al., 2020). Parents performed all these therapeutic techniques throughout the child’s waking hours, which may be the main reason for the high efficacy of FMBEAP. The secondary gain of this intervention was an improvement in parent’s self-efficacy. When parents learn how to manage their child’s behaviors and reduce their child’s behavioral excess, their self-efficacy increases. The results showed that parents can learn all these procedures with high acceptability via telehealth. Thus, telehealth can be a valuable method to deliver behavioral treatments to reduce behavioral excesses in children with ASD with acceptable fidelity.
However, if telehealth is to become a viable method for providing services to families, some prerequisites are necessary, including familiarity with internet-based technology, access to high-speed internet, motivation to participate in treatment, and careful implementation of the intervention strategies.
The current study adds to the empirical evidence for the validity of telehealth service-delivery models, but it has several limitations. The fundamental limitation is the lack of a control group. The absence of a control group makes it impossible to separate the effects of the intervention from the effects of other factors, including regression to mean, time or attention on behavioral excesses, and practice effect. Also, the small sample size limits the generalizability of results. Finally, some measures of the study were filled out by the parents, who were not blinded to the purpose of the study.
The results of this study provided support for the feasibility, acceptability, and efficacy of parent-mediated interventions via telehealth to decrease the behavioral excesses of children with ASD. Additionally, we found that providing training to parents from a distance via video-conferencing technology is an effective and valuable service delivery modality. Given the limitations of this study, further large-scale trials controlling for unrelated factors, and measurement-blind approaches are needed to evaluate the reliability of FMBEAP via telehealth. It is also suggested that the effectiveness of FMBEAP via telehealth be tested in a large sample of immigrant families. Additionally, future issues regarding the delivery of parent-implemented intervention via telehealth should focus on strategies most likely to increase parent’s motivation to engage in online interventions. Finally, telehealth is suggested as a valuable method to deliver psychological services to families of children with ASD in some crisis conditions, including infectious disease outbreaks that necessitate social distancing and staying home.
Conclusion
Taken together, the results of this study provide support for feasibility, acceptability, and efficacy of parent-mediated interventions via telehealth to decrease the behavioral excesses of children with ASD. Additionally, we found that providing training to parents from a distance via video-conferencing technology was an effective and useful modality of service delivery. Given the limitations of this study, further large-scale trials controlling for unrelated factors, as well as blinded approaches to measurement, is needed to evaluate the reliability of FMBEAP via telehealth. It is also suggested to test the effectiveness of FMBEAP via telehealth in a large sample of immigrant families. Additionally, future issues regarding the delivery of parent-implemented intervention via telehealth will need to focus on which strategies are most likely to increase parent’s motivation to engage in online interventions. Finally, thelehealth is suggested as a useful method to deliver psychological services to families of children with ASD in some crisis conditions including infectious disease outbreaks that necessitate social distancing and staying home.
Ethical Considerations
Compliance with ethical guidelines
This study was approved by the Ethical Committee of Shahid Beheshti University, Tehran, Iran (Code: IR. ISB. ICBS. 97/1013).
Funding
This research did not receive any grant from funding agencies in the public, commercial, or non-profit sectors.
Authors' contributions
All authors equally contributed to preparing this article.
Conflict of interest
The authors declared no conflict of interest.
Acknowledgments
The authors thank the Center of Excellence in Cognitive Neuropsychology, Institute for Cognitive and Brain Sciences, Shahid Beheshti University, Tehran, Iran, and all the children and parents who participated in this study.
References
Abareshi, Z., Tahmasian, K., Mazaheri, M. A., & Panaghi, L. (2009). [The impact of psychosocial Child Development training program, done through improvement of mother-child interaction, on parental self-efficacy and relationship between mother and child under three (Persian)]. Journal of Research in Psychological Health, 3(3), 49-58. [Link]
Afrooz G, Kamkari K. Tehran-Stanford-Bineh modern intelligence test: Implementation method, scoring and interpretation. Tehran: University of Tehran; 2016.
Aman, M. G., Singh, N. N., Stewart, A. W., & Field, C. J. (1985). The aberrant behavior checklist: A behavior rating scale for the assessment of treatment effects. American Journal of Mental Deficiency, 89(5), 485-491. [DOI:10.1037/t10453-000]
American Psychiatric Association DS. (2013). Diagnostic and statistical manual of mental disorders: DSM-5. Washington, DC: American Psychiatric Association. [DOI:10.1176/appi.books.9780890425596]
Baker, B. L., McIntyre, L. L., Blacher, J., Crnic, K., Edelbrock, C., & Low, C. (2003). Pre-school children with and without developmental delay: Behaviour problems and parenting stress over time. Journal of Intellectual Disability Research: JIDR, 47(Pt 4-5), 217–230. [DOI:10.1046/j.1365-2788.2003.00484.x] [PMID]
Barretto, A., Wacker, D. P., Harding, J., Lee, J., & Berg, W. K. (2006). Using telemedicine to conduct behavioral assessments. Journal of Applied Behavior Analysis, 39(3), 333–340. [DOI:10.1901/jaba.2006.173-04] [PMID]
Bagherian Khosroshahi, S., Pouretemad, H. R., & Khooshabi, K. (2010). The effect of little bird program in decreasing problem behaviors of autistic children. Procedia - Social and Behavioral Sciences, 5, 1166-1170. [DOI:10.1016/j.sbspro.2010.07.254]
Bearss, K., Burrell, T. L., Challa, S. A., Postorino, V., Gillespie, S. E., & Crooks, C., et al. (2018). Feasibility of parent training via telehealth for children with Autism spectrum disorder and disruptive behavior: A demonstration pilot. Journal of Autism and Developmental Disorders, 48(4), 1020–1030. [DOI:10.1007/s10803-017-3363-2] [PMID]
Bearss, K., Johnson, C., Smith, T., Lecavalier, L., Swiezy, N., & Aman, M., et al. (2015). Effect of parent training vs parent education on behavioral problems in children with autism spectrum disorder: A randomized clinical trial. JAMA, 313(15), 1524–1533. [DOI:10.1001/jama.2015.3150] [PMID]
Benish, S. G., Quintana, S., & Wampold, B. E. (2011). Culturally adapted psychotherapy and the legitimacy of myth: A direct-comparison meta-analysis. Journal of Counseling Psychology, 58(3), 279–289. [DOI:10.1037/a0023626] [PMID]
Belfer, M. L., & Saxena, S. (2006). WHO Child Atlas project. Lancet (London, England), 367(9510), 551–552. [DOI:10.1016/S0140-6736(06)68199-3] [PMID]
Bello-Mojeed, M. A., Omigbodun, O. O., Ogun, O. C., Adewuya, A. O., & Adedokun, B. (2013). The relationship between the pattern of impairments in autism spectrum disorder and maternal psychosocial burden of care. OA Autism, 1(1), 4. [Link]
Bodfish, J. W., Symons, F. J., Parker, D. E., & Lewis, M. H. (2000). Varieties of repetitive behavior in Autism: Comparisons to mental retardation. Journal of Autism and Developmental Disorders, 30(3), 237–243. [DOI:10.1023/A:1005596502855] [PMID]
Boyd, B. A., McDonough, S. G., & Bodfish, J. W. (2012). Evidence-based behavioral interventions for repetitive behaviors in Autism. Journal of Autism and Developmental Disorders, 42(6), 1236–1248. [DOI:10.1007/s10803-011-1284-z] [PMID]
Brookman-Frazee, L., Stahmer, A., Baker-Ericzén, M. J., & Tsai, K. (2006). Parenting interventions for children with autism spectrum and disruptive behavior disorders: Opportunities for cross-fertilization. Clinical Child and Family Psychology Review, 9(3-4), 181–200. [DOI:10.1007/s10567-006-0010-4] [PMID]
Carter, A. S., Messinger, D. S., Stone, W. L., Celimli, S., Nahmias, A. S., & Yoder, P. (2011). A randomized controlled trial of Hanen’s “More Than Words” in toddlers with early autism symptoms. Journal of Child Psychology and Psychiatry, and Allied Disciplines, 52(7), 741–752. [DOI:10.1111/j.1469-7610.2011.02395.x] [PMID]
Castro, F. G., Barrera, M., Jr, & Holleran Steiker, L. K. (2010). Issues and challenges in the design of culturally adapted evidence-based interventions. Annual Review of Clinical Psychology, 6, 213–239. [DOI:10.1146/annurev-clinpsy-033109-132032] [PMID]
Dudding, C. C. (2009). Digital videoconferencing: Applications across the disciplines. Communication Disorders Quarterly, 30(3), 178-182. [DOI:10.1177/1525740108327449]
Dumka, L. E., Stoerzinger, H. D., Jackson, K. M., & Roosa, M. W. (1996). Examination of the cross-cultural and cross-language equivalence of the parenting self-agency measure. National Council on Family Relations, 45(2), 216-222. [DOI:10.2307/585293]
Ghorban, H., Sedigheh, R. D., Marzieh, G., & Yaghoob, G. (2013).Effectiveness of therapeutic horseback riding on social skills of children with autism spectrum disorder in Shiraz, Iran. Journal of Education and Learning, 2(3), 27-38. [DOI:10.5539/jel.v2n3p79]
Grahame, V., Brett, D., Dixon, L., McConachie, H., Lowry, J., & Rodgers, J., et al. (2015). Managing repetitive behaviours in young children with autism spectrum disorder (ASD): Pilot randomised controlled trial of a new parent group intervention. Journal of Autism and Developmental Disorders, 45(10), 3168–3182. [DOI:10.1007/s10803-015-2474-x] [PMID]
Graziano, A. M., & Diament, D. M. (1992). Parent behavioral training. An examination of the paradigm. Behavior Modification, 16(1), 3–38. [DOI:10.1177/01454455920161001] [PMID]
Green, J., Charman, T., McConachie, H., Aldred, C., Slonims, V., & Howlin, P., et al. (2010). Parent-mediated communication-focused treatment in children with autism (PACT): A randomised controlled trial. Lancet (London, England), 375(9732), 2152–2160. [DOI:10.1016/S0140-6736(10)60587-9] [PMID]
Hamad, C. D., Serna, R. W., Morrison, L., & Fleming, R. (2010). Extending the reach of early intervention training for practitioners: A preliminary investigation of an online curriculum for teaching behavioral intervention knowledge in autism to families and service providers. Infants and Young Children, 23(3), 195–208. [DOI:10.1097/IYC.0b013e3181e32d5e] [PMID]
Howroyd, C., & Peeters, T. (2007). Parent participation in early intervention with software-assisted guidance from AutismPro. Good Autism Practice (GAP), 8(2), 31-36. [Link]
Iland, E. D., Weiner, I., & Murawski, W. W. (2012). Obstacles faced by Latina mothers of children with autism. California Journal of Health Promotion, 10(SI-Latino), 25-36.
Jang, J., Dixon, D. R., Tarbox, J., Granpeesheh, D., Kornack, J., & de Nocker, Y. (2012). Randomized trial of an eLearning program for training family members of children with autism in the principles and procedures of applied behavior analysis. Research in Autism Spectrum Disorders, 6(2), 852-856. [DOI:10.1016/j.rasd.2011.11.004]
Johnson, C. R., Handen, B. L., Butter, E., Wagner, A., Mulick, J., & Sukhodolsky D. G., et al. (2007). Development of a parent training program for children with pervasive developmental disorders. Behavioral Interventions, 22(3), 201-221. [DOI:10.1002/bin.237]
Lecavalier, L., Leone, S., & Wiltz, J. (2006). The impact of behaviour problems on caregiver stress in young people with autism spectrum disorders. Journal of Intellectual Disability Research: JIDR, 50(Pt 3), 172–183. [DOI:10.1111/j.1365-2788.2005.00732.x] [PMID]
Leekam, S. R., Prior, M. R., & Uljarevic, M. (2011). Restricted and repetitive behaviors in autism spectrum disorders: A review of research in the last decade. Psychological Bulletin, 137(4), 562–593. [DOI:10.1037/a0023341] [PMID]
Lindgren, S., Wacker, D., Suess, A., Schieltz, K., Pelzel, K., & Kopelman, T., et al. (2016). Telehealth and Autism: Treating challenging behavior at lower cost. Pediatrics, 137(Suppl 2), S167–S175. [DOI:10.1542/peds.2015-2851O] [PMID]
Loftin, R. L., Odom, S. L., & Lantz, J. F. (2008). Social interaction and repetitive motor behaviors. Journal of Autism and Developmental Disorders, 38(6), 1124–1135. [DOI:10.1007/s10803-007-0499-5] [PMID]
Matson JL, Mahan S, Hess JA, Fodstad JC, Neal D. (2010). Progression of challenging behaviors in children and adolescents with autism spectrum disorders as measured by the autism spectrum disorders-problem behaviors for children (ASD-PBC). Research in Autism Spectrum Disorders, 4(3), 400-404. [DOI:10.1016/j.rasd.2009.10.010]
Magaña, S., Lopez, K., & Machalicek, W. (2017). Parents Taking Action: A psycho-educational intervention for latino parents of children with Autism spectrum disorder. Family Process, 56(1), 59–74. [DOI:10.1111/famp.12169] [PMID]
Mohajeri, A., Pourtemad, H., Shokri, O., & Khoshabi, K. (2013). [The effectiveness of parent-child interaction therapy on the parenting self-efficacy of mothers of children with high self-reactivity (Persian)]. Journal of Applied Psychology, 7(1), 21-38. [Link]
Pierce, K., & Courchesne, E. (2001). Evidence for a cerebellar role in reduced exploration and stereotyped behavior in autism. Biological Psychiatry, 49(8), 655–664. [DOI:10.1016/S0006-3223(00)01008-8] [PMID]
Taylor, T. K., Webster-Stratton, C., Feil, E. G., Broadbent, B., Widdop, C. S., & Severson, H. H. (2008). Computer-based intervention with coaching: An example using the incredible years program. Cognitive Behaviour Therapy, 37(4), 233–246.[DOI:10.1080/16506070802364511] [PMID]
Turner, J. W. (2003). Telemedicine: Expanding healthcare into virtual environments. In T. L. Thompson, A. D. Dorsey, K. I. Miller & R. Parrott (Eds), Handbook of health communication (pp. 141-161). Mahwah, NJ: Lawrence Erlbaum Associates. [Link]
Rayner, C., Denholm, C., & Sigafoos, J. (2009). Video-based intervention for individuals with autism: Key questions that remain unanswered. Research in Autism Spectrum Disorders, 3(2), 291-303. [DOI:10.1016/j.rasd.2008.09.001]
Roid, G., Nellis, L., & McLellan, M. (2003). Assessment with the leiter international performance scale--revised and the S-BIT. In R. S. McCallum (Ed.), Handbook of nonverbal assessment (pp. 113–140). New York: Kluwer Academic/Plenum Publishers. [DOI:10.1007/978-1-4615-0153-4_6]
Shiri, E., Pouretemad, H., Fathabadi, J., & Narimani, M. (2020). A pilot study of family-based management of behavioral excesses in young Iranian children with autism spectrum disorder. Asian Journal of Psychiatry, 47, 101845. [DOI:10.1016/j.ajp.2019.101845] [PMID]
Simacek, J., Dimian, A. F., & McComas, J. J. (2017). Communication intervention for young children with severe neurodevelopmental disabilities via telehealth. Journal of Autism and Developmental Disorders, 47(3), 744–767. [DOI:10.1007/s10803-016-3006-z] [PMID]
Sparrow, S. S. (2011). Vineland adaptive behavior scales: Survey form manual: Reference work entry. In J. S. Kreutzer., J. DeLuca ., B. Caplan (Eds.), Encyclopedia of Clinical Neuropsychology (pp. 2618-2621). Berlin: Springer. [Link]
Suess, A. N., Wacker, D. P., Schwartz, J. E., Lustig, N., & Detrick, J. (2016). Preliminary evidence on the use of telehealth in an outpatient behavior clinic. Journal of Applied Behavior Analysis, 49(3), 686–692. [DOI:10.1002/jaba.305] [PMID]
Sue, S. (1998). In search of cultural competence in psychotherapy and counseling. The American Psychologist, 53(4), 440–448.[DOI:10.1037/0003-066X.53.4.440] [PMID]
Sue, S., Fujino, D. C., Hu, L. T., Takeuchi, D. T., & Zane, N. W. (1991). Community mental health services for ethnic minority groups: A test of the cultural responsiveness hypothesis. Journal of Consulting and Clinical Psychology, 59(4), 533–540. [DOI:10.1037/0022-006X.59.4.533] [PMID]
Sigafoos, J., Green, V. A., Payne, D., O’Reilly, M. F., & Lancioni, G. E. (2009). A classroom-based antecedent intervention reduces obsessive-repetitive behavior in an adolescent with Autism. Clinical Case Studies, 8(1), 3-13. [DOI:10.1177/1534650108327475]
Symon, J. B. (2001). Parent education for Autism: Issues in providing services at a distance. Journal of Positive Behavior Interventions, 3(3), 160-174. [DOI:10.1177/109830070100300304]
Szatmari, P., Georgiades, S., Bryson, S., Zwaigenbaum, L., Roberts, W., & Mahoney, W., et al. (2006). Investigating the structure of the restricted, repetitive behaviours and interests domain of autism. Journal of Child Psychology and Psychiatry, and Allied Disciplines, 47(6), 582–590. [DOI:10.1111/j.1469-7610.2005.01537.x] [PMID]
Tawakoli, M., Bagholi, H., Qamat Boland, H., Bovalhari, J., & Birshak, B. (2000). [Normization of the contextualization form of Vineland adaptive behavior scale in Iran (Persian)]. Iranian Journal of Psychiatry, 20, 27-36. [Link]
Vigil, D. C., & Hwa-Froelich, D. A. (2004). Interaction styles in minority caregivers: Implications for intervention. Communication Disorders Quarterly, 25(3), 119-126. [DOI:10.1177/15257401040250030301]
Vismara, L. A., Young, G. S., & Rogers, S. J. (2012). Telehealth for expanding the reach of early autism training to parents. Autism Research and Treatment, 2012, 121878. [DOI:10.1155/2012/121878] [PMID]
Wacker, D. P., Lee, J. F., Dalmau, Y. C., Kopelman, T. G., Lindgren, S. D., & Kuhle, J., et al. (2013). Conducting functional analyses of problem behavior via telehealth. Journal of applied Behavior Analysis, 46(1), 31–46. [DOI:10.1002/jaba.29] [PMID]
Wacker, D. P., Lee, J. F., Padilla Dalmau, Y. C., Kopelman, T. G., Lindgren, S. D., & Kuhle, J., et al. (2013). Conducting functional communication training via telehealth to reduce the problem behavior of young children with Autism. Journal of Developmental and Physical Disabilities, 25(1), 35–48. [DOI:10.1007/s10882-012-9314-0] [PMID]
Type of Study: Original Research Article |
Subject:
Family and group therapy
Received: 2024/09/10 | Accepted: 2024/11/27 | Published: 2025/01/1
Received: 2024/09/10 | Accepted: 2024/11/27 | Published: 2025/01/1
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |