Volume 5, Issue 3 (Summer 2017-- 2017)
PCP 2017, 5(3): 211-216 |
Back to browse issues page
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Sadeghi S, Dolatshahi B, Pourshahbaz A, Zarei M, Kami M. Relationship Between Traumatic Experiences and Somatic Symptoms Severity in Students. PCP 2017; 5 (3) :211-216
URL: http://jpcp.uswr.ac.ir/article-1-465-en.html
URL: http://jpcp.uswr.ac.ir/article-1-465-en.html
1- Department of Clinical Psychology, University of Social Welfare and Rehabilitation Sciences, Tehran, Iran.
2- Department of Clinical Psychology, University of Social Welfare and Rehabilitation Sciences, Tehran, Iran. ,sadeghishahin97@yahoo.com
2- Department of Clinical Psychology, University of Social Welfare and Rehabilitation Sciences, Tehran, Iran. ,
Full-Text [PDF 589 kb]
(2837 Downloads)
| Abstract (HTML) (6741 Views)
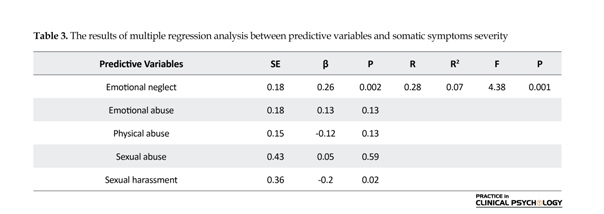
variables, emotional neglect explains the highest proportion of variance, and according to β value, it is the strongest predictor of somatic symptoms severity.
4. Discussion
The goal of the present study was to examine the relationship between traumatic experiences and somatic symptoms severity among the students at the University of Social Welfare and Rehabilitation Sciences. The findings indicated a positive association between traumatic experiences and somatic symptoms severity; this is consistent with the findings of Näring & Nijenhuis (2005) who found a positive relationship between traumatic experiences and somatoform dissociation. In addition, in line with the results of the present study, Bradford et al. (2012) found a positive association between different forms of traumatic experiences and the development of Irritable Bowel Syndrome (IBS). Moreover, Roelofs et al. (2005) indicated that conversion symptoms may result from early-life and also later negative events.
Early life traumatic experiences increase the likelihood of drug abuse and poor mental and physical health during adulthood (Mersky, Topitzes, & Reynolds, 2013). It has also been shown that a reported history of sexual abuse is significantly related to an increase in somatization, illness anxiety, and healthcare utilization (Stein et al., 2004). Papers published in clinical journals on such conditions as anxiety, depression, chronic fatigue syndrome, fibromyalgia, chronic pain, IBS, and syndromes characterized by multifold somatic symptoms related to psychological distress, often contained a possible association with childhood abuse (Springer, Sheridan, Kuo, & Carnes, 2007).
In the present study, traumatic experiences included five subscales: emotional neglect, emotional abuse, physical abuse, sexual harassment, and sexual abuse. Among these subscales, emotional neglect was the sole predictor of somatic symptoms severity; this is consistent with the findings of Schimmenti et al. and Spertus et al. indicating that early life experiences of emotional neglect predict the severity of current psychiatric symptoms.
Previous findings have also shown that women with somatization disorder who have experienced sexual abuse or emotional neglect in their childhood were more likely to grab attention only when they were sick (Çolak, 2014). Moreover, children who were emotionally neglected may not have learned how to cope with negative feelings in family relationships. Therefore, these feelings may be perceived as a source of pressure; difficulty in identifying, tolerating, and modulating these feelings may gradually lead to pathology (Springer et al., 2007). Through their behavior, permissive or emotionally abusing parents send the message to their children that their core self is disappointing because they are not good enough or they do not truly deserve attention and love. Regarding emotional neglect, previous findings show that how shame and other overwhelming feelings are related to childhood abuse that leads to dissociative tendencies in the adulthood (Wright, Crawford, & Del Castillo, 2009).
Consistent with the salient role of emotional neglect found in the present study, Gokten et al. showed that children with attention deficiency/hyperactivity disorder frequently experienced physical and emotional abuse than their healthy counterparts; however, healthy children were more likely to be neglected (Sari Gokten, Saday Duman, Soylu, & Uzun, 2016).
Contrary to our expectations, a negative relationship was found between physical abuse and somatic symptoms severity. Research has shown that seeing other children who have been victims of abuse may protect a child against humiliation and anger; perhaps, this could help children reduce the feelings of being guilty or deviant. This highlights the importance of the way people perceive unpleasant early experiences; this perception is affected by culture, norms, or abusers’ excuses, and may influence the way victims report an experience or are affected by it (Mc Elroy & Hevey, 2014).
Overall, the research shows that patients with a history of abuse show higher healthcare utilization and report more symptoms than those without these experiences (Bradford et al., 2012). The present study also had some practical implications; the study results indicated the importance of traumatic experiences and somatic symptoms in the mental health of students. This can increase parents’ and teachers’ awareness about the long-term harmful effects of traumatic experiences (including emotional mistreatment) on children’s mental health. In addition, the study results can help researchers and clinicians consider traumatic experiences as a risk factor for the development of mental disorders, including somatic symptoms.
Among the limitations of the present study was the sample that only comprised of students at the University of Social Welfare and Rehabilitation Sciences. Therefore, caution should be exercised in generalizing the study results to non-student populations. In addition, the TEC is a checklist comprising of open-ended questions that, if administered along with an interview, can reveal precise information about traumatic experiences. Future studies are suggested to examine the study variables more precisely and make these variables more clear. It is also suggested that the study variables be studied along with clinical samples in order to obtain more information on diagnosis and treatment procedures.
Acknowledgments
This article is the result of Shahin Sadeghi´s MSc. dissertation in clinical psychology at University of Social Welfare and Rehabilitation Sciences. We wish to sincerely thank all those who helped us complete this project, including the students at the University of Social Welfare and Rehabilitation Sciences who gave us their time and support.
Conflict of Interest
The authors declared no conflicts of interest.
References
Bradford, K., Shih, W., Videlock, E. J., Presson, A. P., Naliboff, B. D., Mayer, E. A., et al. (2012). Association between early adverse life events and irritable bowel syndrome. Clinical Gastroenterology and Hepatology, 10(4), 385–90.doi: 10.1016/j.cgh.2011.12.018
Brown, M. J., Masho, S. W., Perera, R. A., Mezuk, B., & Cohen, S. A. (2015). Sex and sexual orientation disparities in adverse childhood experiences and early age at sexual debut in the United States: Results from a nationally representative sample. Child Abuse & Neglect, 46, 89–102. doi: 10.1016/j.chiabu.2015.02.019
Chalavi, S., Vissia, E. M., Giesen, M. E., Nijenhuis, E. R. S., Draijer, N., Cole, J. H., et al. (2014). Abnormal hippocampal morphology in dissociative identity disorder and post-traumatic stress disorder correlates with childhood trauma and dissociative symptoms. Human Brain Mapping, 36(5), 1692–704. doi: 10.1002/hbm.22730
Çolak, T. S. (2014). Somatic expression of psychological problems (somatization): Examination with structural equation model. International Journal of Psychology and Educational Studies, 1(1), 8–14. doi: 10.17220/ijpes.2014.01.003
Debowska, A., & Boduszek, D. (2017). Child abuse and neglect profiles and their psychosocial consequences in a large sample of incarcerated males. Child Abuse & Neglect, 65, 266–77. doi: 10.1016/j.chiabu.2016.12.003
Dijkstra-Kersten, S. M. A., Sitnikova, K., van Marwijk, H. W. J., Gerrits, M. M. J. G., van der Wouden, J. C., Penninx, B. W. J. H., et al. (2015). Somatisation as a risk factor for incident depression and anxiety. Journal of Psychosomatic Research, 79(6), 614–9. doi: 10.1016/j.jpsychores.2015.07.007
Dimsdale, J. E., Creed, F., Escobar, J., Sharpe, M., Wulsin, L., Barsky, A., et al. (2013). Somatic symptom disorder: An important change in DSM. Journal of Psychosomatic Research, 75(3), 223–8. doi: 10.1016/j.jpsychores.2013.06.033
Gierk, B., Kohlmann, S., Toussaint, A., Wahl, I., Brünahl, C. A., Murray, A. M., et al. (2015). Assessing somatic symptom burden: A psychometric comparison of the Patient Health Questionnaire—15 (PHQ-15) and the Somatic Symptom Scale—8 (SSS-8). Journal of Psychosomatic Research, 78(4), 352–5. doi: 10.1016/j.jpsychores.2014.11.006
Han, C., Pae, C. U., Patkar, A. A., Masand, P. S., Kim, K. W., Joe, S. H., et al. (2009). Psychometric properties of the patient health questionnaire-15 (PHQ-15) for measuring the somatic symptoms of psychiatric outpatients. Psychosomatics, 50(6), 580–5. doi: 10.1176/appi.psy.50.6.580
Konnopka, A., Kaufmann, C., König, H.-H., Heider, D., Wild, B., Szecsenyi, J., et al. (2013). Association of costs with somatic symptom severity in patients with medically unexplained symptoms. Journal of Psychosomatic Research, 75(4), 370–5. doi: 10.1016/j.jpsychores.2013.08.011
Lee, S., Creed, F. H., Ma, Y. L., & Leung, C. M. (2015). Somatic symptom burden and health anxiety in the population and their correlates. Journal of Psychosomatic Research, 78(1), 71–6. doi: 10.1016/j.jpsychores.2014.11.012
Mc Elroy, S., & Hevey, D. (2014). Relationship between adverse early experiences, stressors, psychosocial resources and wellbeing. Child Abuse & Neglect, 38(1), 65–75. doi: 10.1016/j.chiabu.2013.07.017
McCall-Hosenfeld, J., Winter, M., Heeren, T., & Liebschutz, J. M. (2014). The association of interpersonal trauma with somatic symptom severity in a primary care population with chronic pain: Exploring the role of gender and the mental health sequelae of trauma. Journal of Psychosomatic Research, 77(3), 196–204. doi: 10.1016/j.jpsychores.2014.07.011
Mersky, J. P., Topitzes, J., & Reynolds, A. J. (2013). Impacts of adverse childhood experiences on health, mental health, and substance use in early adulthood: A cohort study of an urban, minority sample in the U.S. Child Abuse & Neglect, 37(11), 917–25. doi: 10.1016/j.chiabu.2013.07.011
Näring, G., & Nijenhuis, E. R. S. (2005). Relationships between self-reported potentially traumatizing events, psychoform and somatoform dissociation, and absorption, in two non-clinical populations. Australian and New Zealand Journal of Psychiatry, 39(11-12), 982–8. doi: 10.1080/j.1440-1614.2005.01701.x
Nijenhuis, E. R. S., Spinhoven, P., van Dyck, R., van der Hart, O., & Vanderlinden, J. (1998). Degree of somatoform and psychological dissociation in dissociative disorder is correlated with reported trauma. Journal of Traumatic Stress, 11(4), 711–30. doi: 10.1023/a:1024493332751
Nijenhuis, E. R. S., Van der Hart, O., & Kruger, K. (2002). The psychometric characteristics of the Traumatic Experiences Checklist (TEC): First findings among psychiatric outpatients. Clinical Psychology & Psychotherapy, 9(3), 200–10. doi: 10.1002/cpp.332
Reiser, S. J. (2013). Childhood abuse and health anxiety: The roles of attachment and emotion regulation (PhD dissertation). Regina: University of Regina.
Roelofs, K., Spinhoven, P., Sandijck, P., Moene, F. C., & Hoogduin, K. A. L. (2005). The impact of early trauma and recent life-events on symptom severity in patients with conversion disorder. The Journal of Nervous and Mental Disease, 193(8), 508–14. doi: 10.1097/01.nmd.0000172472.60197.4d
Sachs-Ericsson, N., Kendall-Tackett, K., & Hernandez, A. (2007). Childhood abuse, chronic pain, and depression in the national comorbidity survey. Child Abuse & Neglect, 31(5), 531–47. doi: 10.1016/j.chiabu.2006.12.007
Sari Gokten, E., Saday Duman, N., Soylu, N., & Uzun, M. E. (2016). Effects of attention-deficit/hyperactivity disorder on child abuse and neglect. Child Abuse & Neglect, 62, 1–9. doi: 10.1016/j.chiabu.2016.10.007
Schimmenti, A., Maganuco, N. R., La Marca, L., Di Dio, N., Gelsomino, E., & Gervasi, A. M. (2015). Why do I feel so bad: Childhood experiences of emotional neglect, negative affectivity, and adult psychiatric symptoms. Mediterranean Journal of Social Sciences, 6(6), 259. doi: 10.5901/mjss.2015.v6n6s1p259
Shabbeh, Z., Feizi, A., Afshar, H., Hassanzade Kashtali, A., & Adibi, P. (2016). [Identifying the profiles of psychosomatic disorders in an Iranian adult population and their relation to psychological problems (Persian)]. Journal of Mazandaran University of Medical Sciences, 26(137), 82-94.
Spertus, I. L., Yehuda, R., Wong, C. M., Halligan, S., & Seremetis, S. V. (2003). Childhood emotional abuse and neglect as predictors of psychological and physical symptoms in women presenting to a primary care practice. Child Abuse & Neglect, 27(11), 1247–58. doi: 10.1016/j.chiabu.2003.05.001
Springer, K. W., Sheridan, J., Kuo, D., & Carnes, M. (2007). Long-term physical and mental health consequences of childhood physical abuse: Results from a large population-based sample of men and women. Child Abuse & Neglect, 31(5), 517–30. doi: 10.1016/j.chiabu.2007.01.003
Stein, M. B., Lang, A. J., Laffaye, C., Satz, L. E., Lenox, R. J., & Dresselhaus, T. R. (2004). Relationship of sexual assault history to somatic symptoms and health anxiety in women. General Hospital Psychiatry, 26(3), 178–83. doi: 10.1016/j.genhosppsych.2003.11.003
Wright, M. O., Crawford, E., & Del Castillo, D. (2009). Childhood emotional maltreatment and later psychological distress among college students: The mediating role of maladaptive schemas. Child Abuse & Neglect, 33(1), 59–68. doi: 10.1016/j.chiabu.2008.12.007
Xiong, N., Fritzsche, K., Wei, J., Hong, X., Leonhart, R., Zhao, X., et al. (2015). Validation of patient health questionnaire (PHQ) for major depression in Chinese outpatients with multiple somatic symptoms: A multicenter cross-sectional study. Journal of Affective Disorders, 174, 636–43. doi: 10.1016/j.jad.2014.12.042
Full-Text: (5546 Views)
1. Introduction
Patients with Somatic Symptom Disorder (SSD) suffer from impaired thoughts, feelings, and behaviors that cause significant distress or hindrance in normal functioning. In fact, many studies in the field of psychiatric epidemiology have shown that as the number of physical symptoms and maladaptive thoughts, feelings, and behaviors increases, the quality of life decreases (Dimsdale et al., 2013). Patients usually show enduring physical complaints, but somatic examination cannot adequately diagnose the pathology of peripheral organs (Konnopka et al., 2013). Some findings from the community and primary care research on particular symptoms that have not been explained medically indicate that the risk of subsequent pathologies such as depression and anxiety could be elevated by these symptoms (Dijkstra-Kersten et al., 2015).
Several theories have provided an explanation for the high rate of pain symptoms and painful medical conditions related to childhood abuse (Sachs-Ericsson, Kendall-Tackett, & Hernandez, 2007). Empirical studies show that those with traumatic experiences, especially adults who have experienced physical or sexual abuse during childhood, often demonstrate dissociation and medically unexplainable physical symptoms. These findings indicate that somatoform and dissociative symptoms may result from trauma (Nijenhuis, Spinhoven, Van Dyck, Vander Hart, & Vanderlinden, 1998). Harmful experiences include emotional neglect, emotional abuse, physical abuse or severe physical punishment, and sexual abuse (Chalavi et al., 2015).
Research indicates that, each year, 4-16% of children experience physical abuse, 10% experience psychological abuse, 1-15% experience neglect, and 6% experience sexual abuse (Debowska & Boduszek, 2017). Recent estimates have shown that 6 out of 10 people in the general population have experienced at least one unpleasant event during their childhood, and 8.7% (5 or more) report early life traumatic experiences. Early life traumatic experiences are related to higher rates of suicide attempts, taking illicit drugs, smoking, having multiple sexual partners, and late-life depression (Brown, Masho, Perera, Mezuk, & Cohen, 2015). About 2-5% of patients in intensive care units have physical disorders accompanied by anxiety and depression. It is estimated that every year, physical complaints are the reason for about 400 million of all clinic visits in the US. More than half of all outpatient complaints are physical symptoms, one-third of which have no known medical explanation; this category is strongly related to psychiatric disorders, have negative effects on comorbid disorders and quality of life, and lead to functional impairments (Han et al., 2009).
Patients with medically unexplainable symptoms impose direct and indirect costs on the health systems; these costs are heavily dependent on the severity of somatic symptoms (Konnopka et al., 2013). Many studies have shown a relationship between somatization (e.g. development and stability of medically unexplainable physical symptoms) and childhood traumatic experiences. It has been stated that children who were victims of abuse are more likely to demonstrate emotions through physical symptoms. This pattern may continue throughout the person’s life because of a history of emotional trauma accompanied by physical symptoms experienced (Reiser, 2013). McCall-Hosenfeld et al. (2014) found a strong relationship between traumatic experiences and somatic symptoms in both genders.
Stein et al. (2004) also found a strong relationship between sexual trauma and physical symptoms, attitude towards illness, and healthcare utilization in women. Given the high prevalence of somatic symptoms among the student population as well as the impact of traumatic experiences on their mental health, the main goal of the study is to determine the relationship between traumatic experiences and somatic symptoms severity in students. Also, another motivation for conducting the present study is to identify the factors contributing to the development of somatic symptoms and help health care planners and providers improve preventive and treatment programs.
2. Methods
The present study is a cross-sectional one. The statistical population included all students of the University of Social Welfare and Rehabilitation Sciences, Tehran, Iran. The study sample consisted of 264 participants who were selected using a convenience sampling method. Ethical considerations (such as mentally preparing the participants and reassuring them of the confidentiality of personal information) were taken into account, necessary facilities were provided, study objectives were explained to the participants, and their informed consents were obtained. In the next step, the study questionnaires were distributed among the participants. In addition, rewards were offered to motivate the participants.
The inclusion criteria were studying at the university at the time of the study and the willingness of students to participate in the study. Samples who did not meet any of these criteria were removed from the study. The Patient Health Questionnaire Physical Symptoms (PHQ-15) and Traumatic Experiences Checklist (TEC) were used to gather data.
The PHQ-15 is a 15-item questionnaire that was developed to assess somatic symptoms severity during the past 4 weeks. By giving a rating between 0-2 to each item, the respondent indicates the severity of each somatic symptom. This questionnaire has three cut-points, including 5, 10, and 15, indicating low, moderate, and severe somatic symptoms, respectively (Gierk et al., 2015). Good psychometric properties of the PHQ-15 have been shown in various studies. In addition, a Cronbach’s alpha of 0.79 has been reported for the questionnaire (Lee, Creed, Ma, & Leung, 2015).
PHQ-15 has shown good internal consistency. Its positive correlations with 12-Item General Health Questionnaire (GHQ-12) and Beck Depression Inventory (BDI) have indicated its validity. The validity of its Korean version for assessing somatic symptoms severity in the psychiatric outpatient settings has also been demonstrated (Xiong et al., 2015). Research results in Iran show that the validity of the questionnaire using Cronbach’s alpha is 0.92, as well as its sensitivity and specificity are 73.80% and 76.20%, respectively (Shabbeh, Feizi, Afshar, Hassanzade Kashtali, & Adibi, 2016).
The TEC assesses different forms of potentially traumatic experiences. Total score (0-29) indicates the number of traumatic experiences. Composite scores on the trauma domain (0-12) indicate emotional abuse, emotional neglect, sexual harassment, and sexual abuse, physical abuse, and threatening. A value of one is added to the occurrence score for each of the following aspects: presence of the traumatic experience, relationship of the person with the abuser, intensity of the experience, and duration of the traumatic experience. The total composite score on the trauma domain is the sum of the scores on the subscale items (Näring & Nijenhuis, 2005). In addition, the TEC has demonstrated good-to-excellent convergent and criterion validity (Nijenhuis, Van der Hart, & Kruger, 2002). In the present study, the reliability of the TEC was found to be 0.62.
Study data were analyzed using the Pearson correlation coefficient and multiple regression analysis. All analyses were conducted using SPSS software v.20.
3. Results
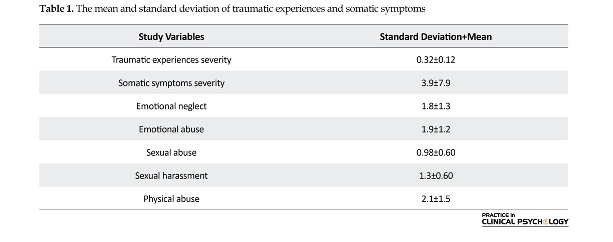
A total of 264 students (50.4% women; 49.6% men; age range: 18-50 years) completed the questionnaires. According to Table 1, the mean and standard deviation of somatic symptoms severity scores are 7.2 and 3.9, respectively. Reports of traumatic experiences were reported by 12% of students, and most of the experiences were in the categories of physical abuse and emotional neglect.
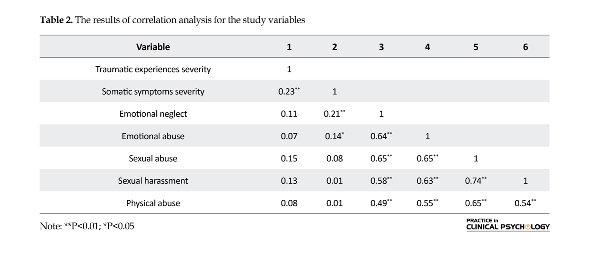
In addition, as you can see in Table 2, there is a significant relationship between early life traumatic experiences and somatic symptoms severity (r=0.23, P<0.01). There is also a significant relationship between the emotional neglect subscale and somatic symptoms severity (r=0.21, P<0.01). According to Table 3, among the five
Patients with Somatic Symptom Disorder (SSD) suffer from impaired thoughts, feelings, and behaviors that cause significant distress or hindrance in normal functioning. In fact, many studies in the field of psychiatric epidemiology have shown that as the number of physical symptoms and maladaptive thoughts, feelings, and behaviors increases, the quality of life decreases (Dimsdale et al., 2013). Patients usually show enduring physical complaints, but somatic examination cannot adequately diagnose the pathology of peripheral organs (Konnopka et al., 2013). Some findings from the community and primary care research on particular symptoms that have not been explained medically indicate that the risk of subsequent pathologies such as depression and anxiety could be elevated by these symptoms (Dijkstra-Kersten et al., 2015).
Several theories have provided an explanation for the high rate of pain symptoms and painful medical conditions related to childhood abuse (Sachs-Ericsson, Kendall-Tackett, & Hernandez, 2007). Empirical studies show that those with traumatic experiences, especially adults who have experienced physical or sexual abuse during childhood, often demonstrate dissociation and medically unexplainable physical symptoms. These findings indicate that somatoform and dissociative symptoms may result from trauma (Nijenhuis, Spinhoven, Van Dyck, Vander Hart, & Vanderlinden, 1998). Harmful experiences include emotional neglect, emotional abuse, physical abuse or severe physical punishment, and sexual abuse (Chalavi et al., 2015).
Research indicates that, each year, 4-16% of children experience physical abuse, 10% experience psychological abuse, 1-15% experience neglect, and 6% experience sexual abuse (Debowska & Boduszek, 2017). Recent estimates have shown that 6 out of 10 people in the general population have experienced at least one unpleasant event during their childhood, and 8.7% (5 or more) report early life traumatic experiences. Early life traumatic experiences are related to higher rates of suicide attempts, taking illicit drugs, smoking, having multiple sexual partners, and late-life depression (Brown, Masho, Perera, Mezuk, & Cohen, 2015). About 2-5% of patients in intensive care units have physical disorders accompanied by anxiety and depression. It is estimated that every year, physical complaints are the reason for about 400 million of all clinic visits in the US. More than half of all outpatient complaints are physical symptoms, one-third of which have no known medical explanation; this category is strongly related to psychiatric disorders, have negative effects on comorbid disorders and quality of life, and lead to functional impairments (Han et al., 2009).
Patients with medically unexplainable symptoms impose direct and indirect costs on the health systems; these costs are heavily dependent on the severity of somatic symptoms (Konnopka et al., 2013). Many studies have shown a relationship between somatization (e.g. development and stability of medically unexplainable physical symptoms) and childhood traumatic experiences. It has been stated that children who were victims of abuse are more likely to demonstrate emotions through physical symptoms. This pattern may continue throughout the person’s life because of a history of emotional trauma accompanied by physical symptoms experienced (Reiser, 2013). McCall-Hosenfeld et al. (2014) found a strong relationship between traumatic experiences and somatic symptoms in both genders.
Stein et al. (2004) also found a strong relationship between sexual trauma and physical symptoms, attitude towards illness, and healthcare utilization in women. Given the high prevalence of somatic symptoms among the student population as well as the impact of traumatic experiences on their mental health, the main goal of the study is to determine the relationship between traumatic experiences and somatic symptoms severity in students. Also, another motivation for conducting the present study is to identify the factors contributing to the development of somatic symptoms and help health care planners and providers improve preventive and treatment programs.
2. Methods
The present study is a cross-sectional one. The statistical population included all students of the University of Social Welfare and Rehabilitation Sciences, Tehran, Iran. The study sample consisted of 264 participants who were selected using a convenience sampling method. Ethical considerations (such as mentally preparing the participants and reassuring them of the confidentiality of personal information) were taken into account, necessary facilities were provided, study objectives were explained to the participants, and their informed consents were obtained. In the next step, the study questionnaires were distributed among the participants. In addition, rewards were offered to motivate the participants.
The inclusion criteria were studying at the university at the time of the study and the willingness of students to participate in the study. Samples who did not meet any of these criteria were removed from the study. The Patient Health Questionnaire Physical Symptoms (PHQ-15) and Traumatic Experiences Checklist (TEC) were used to gather data.
The PHQ-15 is a 15-item questionnaire that was developed to assess somatic symptoms severity during the past 4 weeks. By giving a rating between 0-2 to each item, the respondent indicates the severity of each somatic symptom. This questionnaire has three cut-points, including 5, 10, and 15, indicating low, moderate, and severe somatic symptoms, respectively (Gierk et al., 2015). Good psychometric properties of the PHQ-15 have been shown in various studies. In addition, a Cronbach’s alpha of 0.79 has been reported for the questionnaire (Lee, Creed, Ma, & Leung, 2015).
PHQ-15 has shown good internal consistency. Its positive correlations with 12-Item General Health Questionnaire (GHQ-12) and Beck Depression Inventory (BDI) have indicated its validity. The validity of its Korean version for assessing somatic symptoms severity in the psychiatric outpatient settings has also been demonstrated (Xiong et al., 2015). Research results in Iran show that the validity of the questionnaire using Cronbach’s alpha is 0.92, as well as its sensitivity and specificity are 73.80% and 76.20%, respectively (Shabbeh, Feizi, Afshar, Hassanzade Kashtali, & Adibi, 2016).
The TEC assesses different forms of potentially traumatic experiences. Total score (0-29) indicates the number of traumatic experiences. Composite scores on the trauma domain (0-12) indicate emotional abuse, emotional neglect, sexual harassment, and sexual abuse, physical abuse, and threatening. A value of one is added to the occurrence score for each of the following aspects: presence of the traumatic experience, relationship of the person with the abuser, intensity of the experience, and duration of the traumatic experience. The total composite score on the trauma domain is the sum of the scores on the subscale items (Näring & Nijenhuis, 2005). In addition, the TEC has demonstrated good-to-excellent convergent and criterion validity (Nijenhuis, Van der Hart, & Kruger, 2002). In the present study, the reliability of the TEC was found to be 0.62.
Study data were analyzed using the Pearson correlation coefficient and multiple regression analysis. All analyses were conducted using SPSS software v.20.
3. Results
A total of 264 students (50.4% women; 49.6% men; age range: 18-50 years) completed the questionnaires. According to Table 1, the mean and standard deviation of somatic symptoms severity scores are 7.2 and 3.9, respectively. Reports of traumatic experiences were reported by 12% of students, and most of the experiences were in the categories of physical abuse and emotional neglect.
In addition, as you can see in Table 2, there is a significant relationship between early life traumatic experiences and somatic symptoms severity (r=0.23, P<0.01). There is also a significant relationship between the emotional neglect subscale and somatic symptoms severity (r=0.21, P<0.01). According to Table 3, among the five
variables, emotional neglect explains the highest proportion of variance, and according to β value, it is the strongest predictor of somatic symptoms severity.
4. Discussion
The goal of the present study was to examine the relationship between traumatic experiences and somatic symptoms severity among the students at the University of Social Welfare and Rehabilitation Sciences. The findings indicated a positive association between traumatic experiences and somatic symptoms severity; this is consistent with the findings of Näring & Nijenhuis (2005) who found a positive relationship between traumatic experiences and somatoform dissociation. In addition, in line with the results of the present study, Bradford et al. (2012) found a positive association between different forms of traumatic experiences and the development of Irritable Bowel Syndrome (IBS). Moreover, Roelofs et al. (2005) indicated that conversion symptoms may result from early-life and also later negative events.
Early life traumatic experiences increase the likelihood of drug abuse and poor mental and physical health during adulthood (Mersky, Topitzes, & Reynolds, 2013). It has also been shown that a reported history of sexual abuse is significantly related to an increase in somatization, illness anxiety, and healthcare utilization (Stein et al., 2004). Papers published in clinical journals on such conditions as anxiety, depression, chronic fatigue syndrome, fibromyalgia, chronic pain, IBS, and syndromes characterized by multifold somatic symptoms related to psychological distress, often contained a possible association with childhood abuse (Springer, Sheridan, Kuo, & Carnes, 2007).
In the present study, traumatic experiences included five subscales: emotional neglect, emotional abuse, physical abuse, sexual harassment, and sexual abuse. Among these subscales, emotional neglect was the sole predictor of somatic symptoms severity; this is consistent with the findings of Schimmenti et al. and Spertus et al. indicating that early life experiences of emotional neglect predict the severity of current psychiatric symptoms.
Previous findings have also shown that women with somatization disorder who have experienced sexual abuse or emotional neglect in their childhood were more likely to grab attention only when they were sick (Çolak, 2014). Moreover, children who were emotionally neglected may not have learned how to cope with negative feelings in family relationships. Therefore, these feelings may be perceived as a source of pressure; difficulty in identifying, tolerating, and modulating these feelings may gradually lead to pathology (Springer et al., 2007). Through their behavior, permissive or emotionally abusing parents send the message to their children that their core self is disappointing because they are not good enough or they do not truly deserve attention and love. Regarding emotional neglect, previous findings show that how shame and other overwhelming feelings are related to childhood abuse that leads to dissociative tendencies in the adulthood (Wright, Crawford, & Del Castillo, 2009).
Consistent with the salient role of emotional neglect found in the present study, Gokten et al. showed that children with attention deficiency/hyperactivity disorder frequently experienced physical and emotional abuse than their healthy counterparts; however, healthy children were more likely to be neglected (Sari Gokten, Saday Duman, Soylu, & Uzun, 2016).
Contrary to our expectations, a negative relationship was found between physical abuse and somatic symptoms severity. Research has shown that seeing other children who have been victims of abuse may protect a child against humiliation and anger; perhaps, this could help children reduce the feelings of being guilty or deviant. This highlights the importance of the way people perceive unpleasant early experiences; this perception is affected by culture, norms, or abusers’ excuses, and may influence the way victims report an experience or are affected by it (Mc Elroy & Hevey, 2014).
Overall, the research shows that patients with a history of abuse show higher healthcare utilization and report more symptoms than those without these experiences (Bradford et al., 2012). The present study also had some practical implications; the study results indicated the importance of traumatic experiences and somatic symptoms in the mental health of students. This can increase parents’ and teachers’ awareness about the long-term harmful effects of traumatic experiences (including emotional mistreatment) on children’s mental health. In addition, the study results can help researchers and clinicians consider traumatic experiences as a risk factor for the development of mental disorders, including somatic symptoms.
Among the limitations of the present study was the sample that only comprised of students at the University of Social Welfare and Rehabilitation Sciences. Therefore, caution should be exercised in generalizing the study results to non-student populations. In addition, the TEC is a checklist comprising of open-ended questions that, if administered along with an interview, can reveal precise information about traumatic experiences. Future studies are suggested to examine the study variables more precisely and make these variables more clear. It is also suggested that the study variables be studied along with clinical samples in order to obtain more information on diagnosis and treatment procedures.
Acknowledgments
This article is the result of Shahin Sadeghi´s MSc. dissertation in clinical psychology at University of Social Welfare and Rehabilitation Sciences. We wish to sincerely thank all those who helped us complete this project, including the students at the University of Social Welfare and Rehabilitation Sciences who gave us their time and support.
Conflict of Interest
The authors declared no conflicts of interest.
References
Bradford, K., Shih, W., Videlock, E. J., Presson, A. P., Naliboff, B. D., Mayer, E. A., et al. (2012). Association between early adverse life events and irritable bowel syndrome. Clinical Gastroenterology and Hepatology, 10(4), 385–90.doi: 10.1016/j.cgh.2011.12.018
Brown, M. J., Masho, S. W., Perera, R. A., Mezuk, B., & Cohen, S. A. (2015). Sex and sexual orientation disparities in adverse childhood experiences and early age at sexual debut in the United States: Results from a nationally representative sample. Child Abuse & Neglect, 46, 89–102. doi: 10.1016/j.chiabu.2015.02.019
Chalavi, S., Vissia, E. M., Giesen, M. E., Nijenhuis, E. R. S., Draijer, N., Cole, J. H., et al. (2014). Abnormal hippocampal morphology in dissociative identity disorder and post-traumatic stress disorder correlates with childhood trauma and dissociative symptoms. Human Brain Mapping, 36(5), 1692–704. doi: 10.1002/hbm.22730
Çolak, T. S. (2014). Somatic expression of psychological problems (somatization): Examination with structural equation model. International Journal of Psychology and Educational Studies, 1(1), 8–14. doi: 10.17220/ijpes.2014.01.003
Debowska, A., & Boduszek, D. (2017). Child abuse and neglect profiles and their psychosocial consequences in a large sample of incarcerated males. Child Abuse & Neglect, 65, 266–77. doi: 10.1016/j.chiabu.2016.12.003
Dijkstra-Kersten, S. M. A., Sitnikova, K., van Marwijk, H. W. J., Gerrits, M. M. J. G., van der Wouden, J. C., Penninx, B. W. J. H., et al. (2015). Somatisation as a risk factor for incident depression and anxiety. Journal of Psychosomatic Research, 79(6), 614–9. doi: 10.1016/j.jpsychores.2015.07.007
Dimsdale, J. E., Creed, F., Escobar, J., Sharpe, M., Wulsin, L., Barsky, A., et al. (2013). Somatic symptom disorder: An important change in DSM. Journal of Psychosomatic Research, 75(3), 223–8. doi: 10.1016/j.jpsychores.2013.06.033
Gierk, B., Kohlmann, S., Toussaint, A., Wahl, I., Brünahl, C. A., Murray, A. M., et al. (2015). Assessing somatic symptom burden: A psychometric comparison of the Patient Health Questionnaire—15 (PHQ-15) and the Somatic Symptom Scale—8 (SSS-8). Journal of Psychosomatic Research, 78(4), 352–5. doi: 10.1016/j.jpsychores.2014.11.006
Han, C., Pae, C. U., Patkar, A. A., Masand, P. S., Kim, K. W., Joe, S. H., et al. (2009). Psychometric properties of the patient health questionnaire-15 (PHQ-15) for measuring the somatic symptoms of psychiatric outpatients. Psychosomatics, 50(6), 580–5. doi: 10.1176/appi.psy.50.6.580
Konnopka, A., Kaufmann, C., König, H.-H., Heider, D., Wild, B., Szecsenyi, J., et al. (2013). Association of costs with somatic symptom severity in patients with medically unexplained symptoms. Journal of Psychosomatic Research, 75(4), 370–5. doi: 10.1016/j.jpsychores.2013.08.011
Lee, S., Creed, F. H., Ma, Y. L., & Leung, C. M. (2015). Somatic symptom burden and health anxiety in the population and their correlates. Journal of Psychosomatic Research, 78(1), 71–6. doi: 10.1016/j.jpsychores.2014.11.012
Mc Elroy, S., & Hevey, D. (2014). Relationship between adverse early experiences, stressors, psychosocial resources and wellbeing. Child Abuse & Neglect, 38(1), 65–75. doi: 10.1016/j.chiabu.2013.07.017
McCall-Hosenfeld, J., Winter, M., Heeren, T., & Liebschutz, J. M. (2014). The association of interpersonal trauma with somatic symptom severity in a primary care population with chronic pain: Exploring the role of gender and the mental health sequelae of trauma. Journal of Psychosomatic Research, 77(3), 196–204. doi: 10.1016/j.jpsychores.2014.07.011
Mersky, J. P., Topitzes, J., & Reynolds, A. J. (2013). Impacts of adverse childhood experiences on health, mental health, and substance use in early adulthood: A cohort study of an urban, minority sample in the U.S. Child Abuse & Neglect, 37(11), 917–25. doi: 10.1016/j.chiabu.2013.07.011
Näring, G., & Nijenhuis, E. R. S. (2005). Relationships between self-reported potentially traumatizing events, psychoform and somatoform dissociation, and absorption, in two non-clinical populations. Australian and New Zealand Journal of Psychiatry, 39(11-12), 982–8. doi: 10.1080/j.1440-1614.2005.01701.x
Nijenhuis, E. R. S., Spinhoven, P., van Dyck, R., van der Hart, O., & Vanderlinden, J. (1998). Degree of somatoform and psychological dissociation in dissociative disorder is correlated with reported trauma. Journal of Traumatic Stress, 11(4), 711–30. doi: 10.1023/a:1024493332751
Nijenhuis, E. R. S., Van der Hart, O., & Kruger, K. (2002). The psychometric characteristics of the Traumatic Experiences Checklist (TEC): First findings among psychiatric outpatients. Clinical Psychology & Psychotherapy, 9(3), 200–10. doi: 10.1002/cpp.332
Reiser, S. J. (2013). Childhood abuse and health anxiety: The roles of attachment and emotion regulation (PhD dissertation). Regina: University of Regina.
Roelofs, K., Spinhoven, P., Sandijck, P., Moene, F. C., & Hoogduin, K. A. L. (2005). The impact of early trauma and recent life-events on symptom severity in patients with conversion disorder. The Journal of Nervous and Mental Disease, 193(8), 508–14. doi: 10.1097/01.nmd.0000172472.60197.4d
Sachs-Ericsson, N., Kendall-Tackett, K., & Hernandez, A. (2007). Childhood abuse, chronic pain, and depression in the national comorbidity survey. Child Abuse & Neglect, 31(5), 531–47. doi: 10.1016/j.chiabu.2006.12.007
Sari Gokten, E., Saday Duman, N., Soylu, N., & Uzun, M. E. (2016). Effects of attention-deficit/hyperactivity disorder on child abuse and neglect. Child Abuse & Neglect, 62, 1–9. doi: 10.1016/j.chiabu.2016.10.007
Schimmenti, A., Maganuco, N. R., La Marca, L., Di Dio, N., Gelsomino, E., & Gervasi, A. M. (2015). Why do I feel so bad: Childhood experiences of emotional neglect, negative affectivity, and adult psychiatric symptoms. Mediterranean Journal of Social Sciences, 6(6), 259. doi: 10.5901/mjss.2015.v6n6s1p259
Shabbeh, Z., Feizi, A., Afshar, H., Hassanzade Kashtali, A., & Adibi, P. (2016). [Identifying the profiles of psychosomatic disorders in an Iranian adult population and their relation to psychological problems (Persian)]. Journal of Mazandaran University of Medical Sciences, 26(137), 82-94.
Spertus, I. L., Yehuda, R., Wong, C. M., Halligan, S., & Seremetis, S. V. (2003). Childhood emotional abuse and neglect as predictors of psychological and physical symptoms in women presenting to a primary care practice. Child Abuse & Neglect, 27(11), 1247–58. doi: 10.1016/j.chiabu.2003.05.001
Springer, K. W., Sheridan, J., Kuo, D., & Carnes, M. (2007). Long-term physical and mental health consequences of childhood physical abuse: Results from a large population-based sample of men and women. Child Abuse & Neglect, 31(5), 517–30. doi: 10.1016/j.chiabu.2007.01.003
Stein, M. B., Lang, A. J., Laffaye, C., Satz, L. E., Lenox, R. J., & Dresselhaus, T. R. (2004). Relationship of sexual assault history to somatic symptoms and health anxiety in women. General Hospital Psychiatry, 26(3), 178–83. doi: 10.1016/j.genhosppsych.2003.11.003
Wright, M. O., Crawford, E., & Del Castillo, D. (2009). Childhood emotional maltreatment and later psychological distress among college students: The mediating role of maladaptive schemas. Child Abuse & Neglect, 33(1), 59–68. doi: 10.1016/j.chiabu.2008.12.007
Xiong, N., Fritzsche, K., Wei, J., Hong, X., Leonhart, R., Zhao, X., et al. (2015). Validation of patient health questionnaire (PHQ) for major depression in Chinese outpatients with multiple somatic symptoms: A multicenter cross-sectional study. Journal of Affective Disorders, 174, 636–43. doi: 10.1016/j.jad.2014.12.042
Type of Study: Original Research Article |
Subject:
Cognitive behavioral
Received: 2017/01/10 | Accepted: 2017/05/1 | Published: 2017/07/1
Received: 2017/01/10 | Accepted: 2017/05/1 | Published: 2017/07/1
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |